Imagine waking up to find tiny, fluid-filled blisters appearing across the palms of your hands, between your fingers, or along the soles of your feet. They itch relentlessly, burn with fierce intensity, and make even the simplest daily tasks feel like a monumental struggle. Typing on a keyboard, holding a steering wheel, or simply tying your shoelaces suddenly becomes an agonising ordeal. Worse still, these frustrating flare-ups have a habit of returning, often striking at the most inconvenient moments imaginable. If you've ever experienced this distressing cycle of itching, blistering, and peeling, you might be dealing with a widespread but frequently misunderstood skin condition known as dyshidrotic eczema.
Living with this condition can feel incredibly isolating, but you're far from alone. Millions of people worldwide struggle with the unpredictable nature of these outbreaks. While the exact origins of the condition can sometimes seem elusive, modern dermatology and natural skincare science have made tremendous strides in understanding how to manage, soothe, and prevent these painful episodes. By learning to identify your personal triggers and adopting a deeply nourishing skincare routine, you can reclaim control over your skin's health and find lasting relief from the persistent discomfort.

Key takeaways if you're short on time
- Intensely itchy blisters, primarily affecting the palms of the hands, sides of the fingers, and soles of the feet.
- Chronic and recurring nature, meaning the condition often returns in cycles, requiring long-term management strategies.
- Triggered by stress and allergens, making lifestyle adjustments and careful observation vital for preventing future flare-ups.
- Proper hydration is essential, demanding deeply nourishing natural oils and creams to repair the compromised skin barrier.
- Gentle cleansing matters, as harsh, heavily fragranced chemicals strip the skin of its natural defences and exacerbate inflammation.
What Exactly Is Dyshidrotic Eczema?
Dyshidrotic eczema, sometimes referred to in medical literature as pompholyx or dyshidrotic dermatitis, is an inflammatory skin condition characterised by the sudden eruption of small, intensely itchy blisters. The term "pompholyx" originates from the ancient Greek word for bubble, which perfectly describes the appearance of these tiny, fluid-filled vesicles. Unlike other forms of dermatitis that might appear anywhere on the body, this specific condition is strictly confined to the hands and feet. The blisters are typically pale, deeply seated within the skin, and can merge to form larger, highly painful areas of inflammation.
One of the most challenging aspects of dyshidrotic eczema is its chronic and cyclical nature. The condition rarely appears just once; rather, it tends to flare up repeatedly over months or even years. Patients often experience periods of complete remission when their skin looks entirely normal, only to be suddenly hit by a severe outbreak. This unpredictability can take a significant emotional toll, leading to anxiety and frustration. Understanding the underlying mechanisms of the condition is the first crucial step towards breaking this exhausting cycle.

The condition is particularly prevalent among individuals who already have a genetic predisposition to atopic diseases. If you have a history of asthma, hay fever, or other types of allergic reactions, your immune system is already primed to overreact to environmental stimuli. Consequently, your skin barrier may be inherently weaker, making it far more susceptible to the inflammatory cascade that results in dyshidrotic eczema. Recognising this connection helps you create a comprehensive treatment plan that addresses not just the external symptoms, but the internal immune responses as well.
How to Recognise the Symptoms of Dyshidrotic Eczema
Identifying dyshidrotic eczema early can drastically improve the effectiveness of your treatment. The condition typically progresses through several distinct stages, each presenting its own unique set of uncomfortable symptoms. Before any visible signs appear on the surface of the skin, many people experience an early warning phase (known medically as a prodrome). During this time, you might notice an unusual tingling, burning, or deep-seated itching sensation in your palms or the soles of your feet. This early warning sign is your body signalling that an inflammatory response is brewing beneath the surface.
Following the initial itching, the hallmark blisters begin to emerge. These vesicles are usually very small—often compared to tapioca pearls—and are filled with clear fluid. Because they form deep within the epidermis, they don't pop easily. In fact, you should never try to burst them, as this can lead to severe secondary bacterial infections and increased pain. As the blisters multiply, the surrounding skin becomes visibly red, swollen, and warm to the touch. The itching during this acute phase can be so severe that it disrupts sleep and concentration.
As the acute phase subsides, the condition transitions into a chronic, healing stage that brings a different kind of discomfort. The blisters eventually dry out, causing the overlying skin to harden, thicken, and peel away in large flakes. This process, known as lichenification, leaves the underlying skin raw, exceptionally dry, and prone to painful fissuring. Deep cracks can form over the joints of the fingers or the heels, making movement excruciating. Learning how to care for dry skin during this peeling phase is absolutely vital to restore elasticity and prevent the cracks from deepening.
Who Is Most Vulnerable? Exploring the Risk Factors
Dyshidrotic eczema doesn't strike at random; there are specific demographic and physiological factors that significantly elevate a person's risk of developing the condition. One of the most prominent risk factors is a pre-existing history of allergies or asthma. Individuals who fall into this category have an immune system that is inherently hyper-reactive. When exposed to even minor environmental irritants, their bodies launch a disproportionate defensive response, which often manifests as severe skin inflammation.
Another major risk factor is a history of contact dermatitis. If your skin is already sensitive to certain metals, chemicals, or cosmetic ingredients, repeated exposure to these substances can eventually trigger a dyshidrotic flare-up. Occupational hazards play a significant role here. Hairdressers, healthcare workers, mechanics, and cleaners who frequently expose their hands to water, harsh detergents, and solvents are exceptionally vulnerable. The constant stripping of the skin's natural lipid barrier leaves the hands defenceless against irritants.
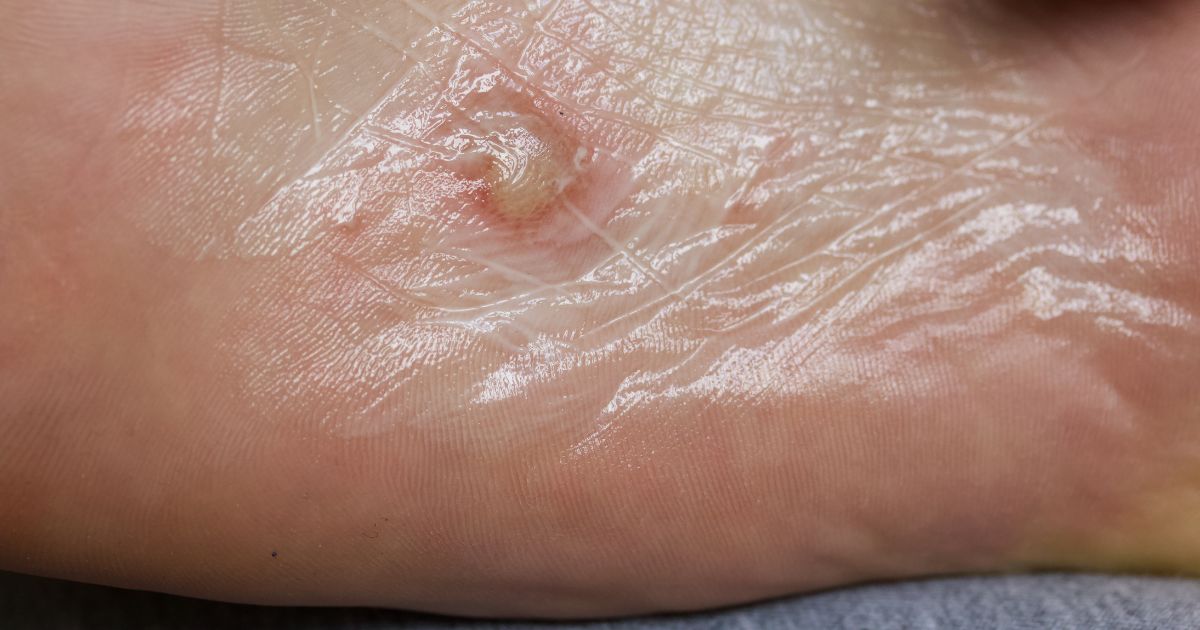
Interestingly, there's also a strong correlation between dyshidrotic eczema and hyperhidrosis, a medical condition characterised by excessive sweating. The constant presence of moisture on the palms and soles can macerate the skin, breaking down its protective outer layer and creating an ideal environment for eczema to thrive. Furthermore, genetics play an undeniable role. If your parents or siblings suffer from eczema, your likelihood of developing the condition is substantially higher, suggesting that structural weaknesses in the skin barrier are inherited traits.
Uncovering the Root Causes Behind the Blisters
While dermatologists can easily diagnose the condition, pinpointing the exact root cause remains a complex challenge. Current medical consensus suggests that dyshidrotic eczema is a multifactorial disease, meaning it arises from a combination of internal vulnerabilities and external triggers. At the core of the issue is an imbalance within the immune system. Certain T-cells within the skin become overactive, releasing inflammatory cytokines that cause fluid to accumulate between the skin cells, ultimately forming the characteristic blisters.
Equally important is the concept of skin barrier dysfunction. Healthy skin acts as a robust brick wall, keeping moisture locked inside and preventing allergens, bacteria, and irritants from penetrating. In people with eczema, this wall is inherently faulty. The skin lacks essential lipids and proteins, such as filaggrin, which are necessary for maintaining structural integrity. When this compromised barrier is exposed to everyday stressors, it simply can't cope, leading to the rapid development of dyshidrotic eczema.
Gentle Cleansing Essentials for Sensitive Skin
Common Triggers That Aggravate Dyshidrotic Eczema
To effectively manage this frustrating condition, you must become a detective in your own life, carefully observing what sets off your symptoms. One of the most universally recognised triggers is psychological stress. In our fast-paced modern world, stress is often unavoidable, but its impact on the skin is profound. When you're stressed, your body releases a surge of cortisol, a hormone that suppresses the immune system's normal functioning and drastically increases systemic inflammation. This internal turmoil frequently manifests externally as a severe dyshidrotic eczema flare-up, creating a vicious cycle where the eczema causes more stress, which in turn worsens the eczema.
Allergies and environmental irritants are equally notorious culprits. Many patients find that their skin reacts violently to specific metals, particularly nickel and cobalt, which are commonly found in everyday items such as jewellery, keys, coins, and even certain mobile phones. Dietary allergens can also play a role; some individuals notice that consuming foods high in nickel, such as chocolate, oats, or certain legumes, exacerbates their symptoms. The cosmetic products you use every day might also be secretly sabotaging your skin. Heavily fragranced soaps, aggressive shampoos, and synthetic lotions can strip away the skin's protective oils. Understanding how to cleanse skin properly without causing micro-damage is a fundamental skill for anyone prone to eczema.
Environmental factors and bodily changes also contribute significantly to the onset of symptoms. Rapid fluctuations in temperature, particularly the transition into hot, humid summer months, can trigger an outbreak. This is closely tied to the issue of excessive sweating. Sweat contains trace amounts of minerals and salts that, when trapped against compromised skin, act as potent irritants. Crucially, while managing sweat is important, you must also be mindful of your skin's natural sebum production. Reading about how to care for oily skin can provide valuable insights into balancing lipid production, ensuring your skin remains protected without becoming a breeding ground for irritation.
Getting a Professional Diagnosis for Your Skin Concerns
While the symptoms of dyshidrotic eczema may seem obvious to those suffering from it, obtaining a formal diagnosis from a qualified dermatologist is absolutely essential. Many other skin conditions, such as fungal infections (like athlete's foot or tinea manuum), palmoplantar psoriasis, and severe contact dermatitis, can mimic the exact appearance of dyshidrotic blisters. Attempting to treat a fungal infection with eczema medication, or vice versa, can lead to disastrous results and prolonged suffering.
During a consultation, a dermatologist will typically conduct a thorough physical examination of the affected areas, taking note of the blister distribution, skin thickness, and any signs of secondary infection. To rule out allergic contact dermatitis, they may recommend comprehensive patch testing. This involves applying small amounts of common allergens to your back and observing the skin's reaction over several days. In some complex cases, they might order blood tests to assess your overall immune function and identify specific IgE antibodies related to environmental allergies.
If the diagnosis remains uncertain, or if the condition proves entirely resistant to standard treatments, the doctor might perform a skin biopsy. This minor procedure involves removing a tiny sample of the affected skin under local anaesthetic. The sample is then examined under a microscope by a dermatopathologist, who can identify the specific cellular changes characteristic of dyshidrotic eczema, thereby confirming the diagnosis and paving the way for a targeted treatment plan.
Effective Treatment Strategies for Dyshidrotic Eczema
The good news for anyone suffering from this condition is that a wide array of treatment options is available. The somewhat frustrating reality, however, is that there's no single "magic bullet." What works miracles for one person might have little to no effect on another. Finding the right treatment protocol usually requires patience, persistence, and a willingness to combine conventional medical interventions with high-quality natural skincare.
Conventional medical treatments generally aim to suppress the immediate inflammatory response. Dermatologists frequently prescribe high-potency topical corticosteroids to rapidly reduce redness, swelling, and the unbearable itch. While effective in the short term, these creams can't be used indefinitely, as they can cause the skin to thin and become even more fragile over time. For intense itching, doctors often recommend oral antihistamines, particularly to help patients sleep through the night. In exceptionally severe, unmanageable cases, doctors might resort to systemic immunosuppressants or phototherapy (controlled exposure to specific wavelengths of ultraviolet light). Interestingly, recent clinical studies have demonstrated that targeted injections of Botulinum toxin A (Botox) into the palms or soles can significantly reduce blistering, primarily by halting the excessive sweating that triggers the condition.

Alongside medical treatments, supporting the skin's structural integrity from the inside out and the outside in is paramount. Incorporating a high-quality barrier repair cream is non-negotiable. For instance, applying the Natural Nourishing Body Cream AtopCare 330 ml provides an immediate surge of moisture, helping to seal the cracked epidermis and shield vulnerable nerve endings from the air. You might also want to explore internal supplements to support tissue regeneration. Learning about the best collagen for hair and skin can be incredibly beneficial, as collagen peptides provide the essential amino acid building blocks your body needs to rebuild the damaged dermal layers.
Deep Nourishment for Eczema-Prone Skin
Building a Daily Care Routine to Prevent Eczema Flare-Ups
Treating an active flare-up is only half the battle; the ultimate goal is to prevent the blisters from returning in the first place. This requires a steadfast commitment to a gentle, protective daily skincare routine. The foundation of this routine is avoiding triggers. If you know that peeling potatoes or washing dishes irritates your hands, you must form a habit of wearing protective gloves. Ideally, wear a thin pair of breathable cotton gloves underneath waterproof rubber or nitrile gloves, as the rubber itself can cause sweating and irritation.
When it comes to hand hygiene, you must abandon standard commercial soaps, which are typically loaded with harsh surfactants like sodium lauryl sulphate (SLS) and artificial fragrances. Instead, transition to a deeply soothing alternative like the Moisturizing Cleansing Foam AtopCare 150 ml. This ensures that you remove dirt and bacteria without stripping away the microscopic lipid layer that your skin desperately needs to heal. Wash your hands with lukewarm water—never hot, as heat stimulates histamine release and intensifies itching—and pat them dry gently with a soft towel rather than rubbing vigorously.
The most critical step in your daily routine is the immediate application of an emollient after every single wash. Within three minutes of drying your hands, you must lock in the residual moisture. Using a rich, botanical blend like the Natural Nurturing Body Oil AtopCare 200 ml provides a protective seal over the skin. Even during periods of remission, when your skin looks perfectly clear, you must maintain this rigorous moisturising schedule. Consistency is the ultimate weapon against chronic skin conditions.
Why Natural Oils Provide Vital Relief for Compromised Skin
When dealing with a compromised skin barrier, the ingredients you apply matter immensely. Synthetic moisturisers often sit on the surface of the skin, creating an artificial barrier that washes away instantly. In contrast, natural, plant-derived oils have a molecular structure that closely mimics human sebum, allowing them to penetrate deeply and repair the skin from within. A comprehensive formulation designed for atopic skin relies on a synergistic blend of these botanical powerhouses.
Sweet almond oil is a fundamental ingredient, renowned for its exceptional regenerative properties and high vitamin E content, which helps protect the skin from oxidative stress. Oat lipid extract is another vital component; oats have been used for centuries to soothe itching and reduce redness, thanks to their potent anti-inflammatory compounds called avenanthramides. Hemp seed oil is equally crucial, as it contains an optimal ratio of omega-3 and omega-6 fatty acids that actively encourage the rebuilding of the epidermal wall. Finally, the inclusion of squalane—a highly stable, plant-derived lipid—provides unparalleled hydration without leaving a heavy, greasy residue.
Advanced natural skincare also uses innovative botanical complexes, such as Emolid® CC, which work in harmony with these base oils to create a breathable, protective film over the skin. This film drastically reduces transepidermal water loss (TEWL), ensuring that the deep layers of the skin remain hydrated throughout the day. By choosing products that are 100% free from parabens, silicones, and artificial colourants, you significantly minimise the risk of provoking an allergic response, giving your skin the peaceful environment it needs to finally heal.
Conclusion: A Comprehensive Approach Is Essential for Success
Conquering dyshidrotic eczema is rarely achieved through a single miracle cream or a one-time medical treatment. It demands a holistic, comprehensive approach that addresses the condition from multiple angles. By diligently identifying and avoiding your personal triggers, you remove the constant source of irritation. By committing to a rigorous daily routine of gentle cleansing and deep, natural moisturisation, you fortify your skin's natural defences. Finally, by managing systemic factors like stress and diet, you calm the internal immune responses that fuel the fire. While the journey to clear skin may require patience and perseverance, the combination of professional medical guidance and high-quality, natural barrier repair offers a highly effective pathway to long-lasting relief and restored comfort.
Frequently asked questions
Is dyshidrotic eczema contagious?
No, dyshidrotic eczema is absolutely not contagious. It's an internal inflammatory and autoimmune response, meaning you can't catch it from someone else, nor can you pass it on to friends or family members through physical contact or shared items.
How long does it take for an eczema flare-up to heal?
The healing timeline is highly individual. Mild flare-ups might resolve within a couple of weeks if treated promptly, whereas severe, chronic episodes can persist for months. Consistent, gentle skincare and strict trigger avoidance are vital for speeding up the recovery process.
Can my diet influence my skin condition?
Yes, diet can play a significant role for some individuals. Foods high in nickel (such as soy, oatmeal, chocolate, and certain nuts) or common allergens like dairy and gluten can trigger systemic inflammation that worsens eczema symptoms in highly sensitive people.
Is it possible to cure this type of eczema completely?
While there's currently no permanent medical cure for dyshidrotic eczema, it's entirely possible to achieve long-term remission. With a dedicated skincare routine, stress management, and trigger avoidance, many people successfully keep their symptoms at bay for years at a time.
Which natural oils are best for managing eczema-prone skin?
The most effective natural oils for compromised skin include sweet almond oil, hemp seed oil, oat lipid, and squalane. These botanical ingredients deeply hydrate, reduce inflammation, and provide the essential fatty acids required to rebuild the skin's protective barrier.
Sources
- Czarnowicki et al. (2015) – Severe atopic dermatitis is characterized by selective expansion of circulating TH2/TC2 and TH22/TC22, but not TH17/TC17, cells within the skin-homing T-cell population.
- Kimber & Dearman (2002) – Allergic contact dermatitis: the cellular effectors.
- Tokura et al. (2018) – Atopic dermatitis as Th2 disease revisited.
- Tatsuno et al. (2015) – TSLP directly interacts with skin-homing Th2 cells highly expressing its receptor to enhance IL-4 production in atopic dermatitis.
- Nakajima et al. (2020) – Anti-TSLP antibodies: targeting a master regulator of type 2 immune responses.
- Imai et al. (2021) – Dupilumab effects on innate lymphoid cell and helper T cell populations in patients with atopic dermatitis.
- Tsoi et al. (2019) – Atopic dermatitis is an IL-13-dominant disease with greater molecular heterogeneity compared to psoriasis.
- Koppes et al. (2016) – Stratum corneum tape stripping: monitoring of inflammatory mediators in atopic dermatitis patients using topical therapy.
- Rafei-Shamsabadi et al. (2019) – Context dependent role of type 2 innate lymphoid cells in allergic skin inflammation.
- Xiong et al. (2022) – Innate lymphoid cells: more than just immune cells.






