Imagine waking early to the sound of your little one crying because they simply can't open their eyes. You rush in to find their eyelashes crusted together by stubborn discharge, the whites of their eyes turned an angry, inflamed red. If this sounds familiar, you're likely dealing with conjunctivitis — one of the most common eye ailments in children. It can trigger instant panic, but understanding the causes and knowing how to respond transforms a stressful morning into a manageable hurdle. In this guide, we'll explore everything you need to know: from spotting early warning signs and distinguishing between types of infection, to implementing effective treatments and preventive measures that keep those bright little eyes healthy and clear.

Key takeaways if you're short on time
- Bacterial infections are the main culprit, responsible for roughly 70% of all childhood cases and typically presenting with thick, yellowish-green discharge that glues the eyelids shut overnight.
- Viral and allergic triggers also play a major role, with viruses causing highly contagious watery discharge, while allergens lead to intense itching and swelling without thick pus.
- Strict household hygiene is vital, as both bacterial and viral forms are highly contagious and spread easily through shared towels, pillowcases, or hand-to-eye contact.
- Managing indoor allergens provides long-term relief, especially when using specialist nanofabric bedding to protect your child's sensitive eyes and airways from dust mites during the night.
- Professional medical advice is essential, particularly if symptoms don't improve within a few days, if your child has severe eye pain, or if their vision becomes blurred.
What Exactly Is Conjunctivitis in Children?
To understand this common ailment, you need to know what the conjunctiva is. The conjunctiva is a thin, virtually transparent mucous membrane lining the inside of the eyelids and covering the sclera — the white part of the eyeball. Under normal conditions, this delicate membrane is barely noticeable. It quietly produces mucus and tears to keep the eye surface lubricated and protected from dust and pathogens.
When this tissue becomes irritated or infected, the tiny blood vessels within it rapidly dilate and swell. This sudden rush of blood gives the eye that alarming bloodshot appearance that worries parents. Conjunctivitis is particularly common in children simply because young ones explore the world with their hands and rarely remember to wash them before rubbing their tired eyes. This unwashed hand-to-eye contact creates the perfect pathway for bacteria, viruses, and allergens to settle directly onto the vulnerable eye surface.
The impact goes beyond colour change. The swelling can cause a gritty feeling, as if a grain of sand is stuck beneath the eyelid. For a young child who can't fully articulate what they're feeling, this is incredibly frustrating and often leads to more eye rubbing — which only worsens the inflammation and spreads the infection further. Understanding this biological response is the first step in approaching treatment with a calm, informed mindset.
Recognising the Tell-tale Symptoms of Conjunctivitis in Children
Spotting an eye infection early makes a real difference in how quickly your child recovers and how effectively you can prevent it from spreading to the rest of the family or their classmates. While the classic "pink eye" appearance is the most recognised symptom, conjunctivitis can actually vary quite a bit depending on the underlying cause. However, there's a core set of symptoms parents should always watch for.

The most immediate sign is pronounced redness in the white of the eye or on the inner eyelid. This is often accompanied by unusual discharge. Depending on the infection, this can range from clear, watery fluid that makes the eye look constantly teary, to thick, sticky, yellowish or greenish pus. It's this thicker discharge that dries and crusts overnight, leading to the morning scenario where the child's eyelids are literally glued shut. For a broader perspective on how these symptoms manifest across different age groups, see our detailed guide on Conjunctivitis in children and adults: everything you need to know.
Beyond the visible redness and discharge, children often complain of a burning or stinging sensation. They might say their eye feels "scratchy" or that something's stuck in it. You may notice their eyelids appear puffy and swollen, sometimes to the point where the eye looks partially closed even when they're fully awake. Increased sensitivity to bright light (photophobia) can also occur, causing them to squint heavily or turn away from windows and lamps. Relentless, intense itching is another hallmark symptom, particularly when the inflammation is driven by an allergic reaction rather than a bacterial or viral infection. Monitoring these nuances will provide essential clues to both you and your GP about which treatment will be most effective.
The Three Main Culprits Behind the Inflammation
To effectively treat and manage this condition, it's vital to understand that not all eye infections are created equal. Studies and paediatric data reveal that conjunctivitis in children is generally triggered by one of three main culprits: bacteria, viruses, or allergens. Each requires a slightly different approach to care.
Bacterial Conjunctivitis: the Sticky, Crusty Invader
Bacterial infections account for the lion's share of childhood cases, representing more than half of all diagnoses. The most frequent bacterial offenders are Haemophilus influenzae, Streptococcus pneumoniae, and occasionally Moraxella catarrhalis. These are the same bacteria often responsible for common childhood ear infections and sinus issues. In fact, it's quite common for a child to develop a bacterial eye infection alongside a painful ear infection, which is why a thorough GP check-up will often include examining the ears too.
When bacteria are the root cause, the hallmark symptom is copious, thick, purulent discharge. This pus is usually yellow or green and continuously oozes from the eye throughout the day. It's this bacterial discharge that leads to severe crusting and gluing of the eyelashes after a night's sleep. Bacterial conjunctivitis usually begins in one eye but can easily spread to the other if the child rubs the infected eye and then touches the healthy one. Because it's highly contagious, immediate intervention and strict hygiene are absolutely essential to contain the spread.
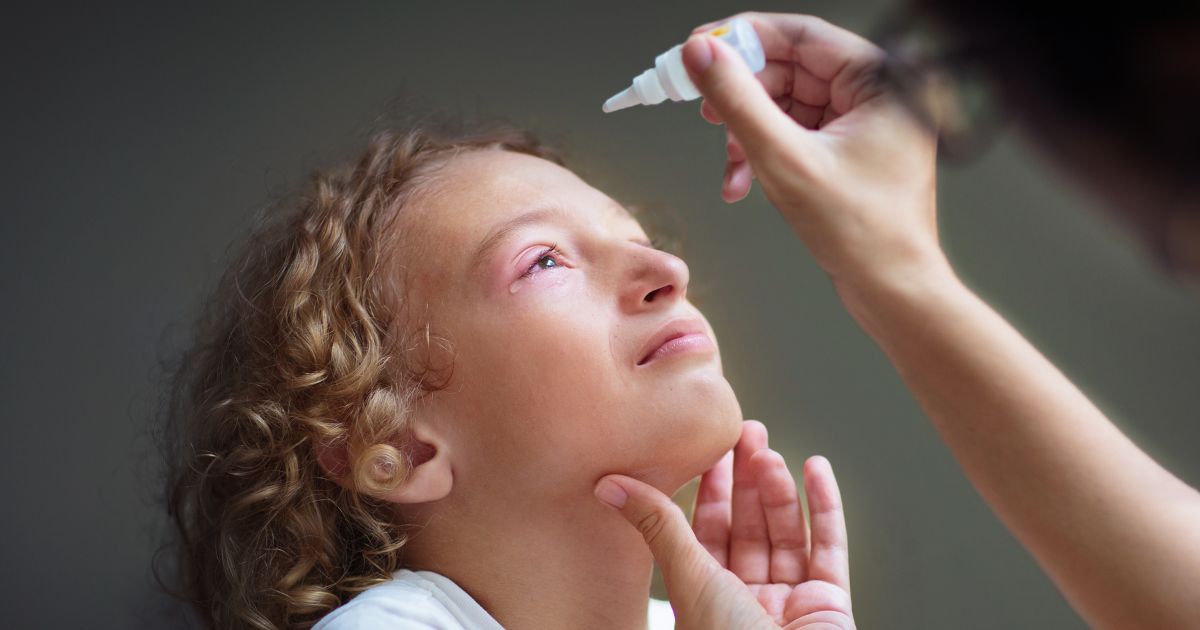
Viral Conjunctivitis: the Watery, Highly Contagious Companion
The second most common form is caused by viruses — very often the same adenoviruses responsible for the common cold, sore throats, and upper respiratory infections. Because the mucous membranes of the nose, throat, and eyes are all interconnected, a child with a runny nose or cough can easily transfer the virus to their eyes by blowing their nose and then rubbing their face.
Unlike the thick pus associated with bacterial infections, viral conjunctivitis typically presents with profuse, clear, watery discharge. The eye may look incredibly red and glassy, and the child might experience severe burning. Viral infections also spread incredibly fast. It's almost guaranteed that if it starts in one eye, it'll migrate to the second within 24 to 48 hours. Alongside the eye symptoms, you might notice swollen lymph nodes — particularly the small nodes just in front of the ears — and they may run a mild fever.
Allergic Conjunctivitis: the Itchy, Seasonal Nuisance
Affecting roughly one in five children, allergic conjunctivitis is a completely different beast. Unlike bacterial and viral forms, this type isn't an infection at all — it's an overreaction of the child's immune system to a harmless environmental substance, such as pollen, pet dander, or dust mites. When the sensitive conjunctiva comes into contact with these allergens, the body releases histamines, which rapidly trigger inflammation, extreme itchiness, and swelling.
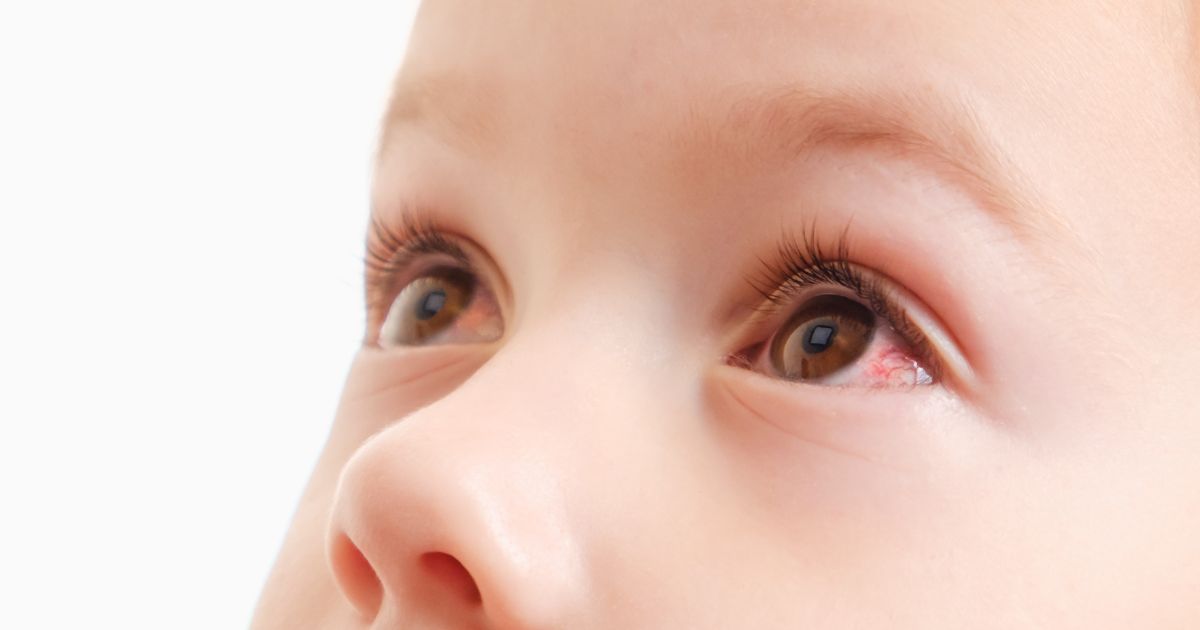
Allergic conjunctivitis almost always affects both eyes simultaneously. The defining characteristic is overwhelming, almost unbearable itchiness that drives children to rub their eyes constantly. The discharge is usually clear and watery, and the condition is frequently accompanied by other classic allergy symptoms: a runny or stuffy nose, relentless sneezing, and a scratchy throat. If you notice these accompanying respiratory signs, you might be looking at Allergic rhinitis symptoms, which often go hand-in-hand with allergic eye inflammation.
The Hidden Danger of Dust Mites in the Bedroom
When discussing allergic conjunctivitis in children, it's impossible to ignore the huge role played by the indoor environment — specifically the child's bedroom. While spring pollen and neighbourhood pets are obvious suspects, one of the most insidious triggers for chronic eye inflammation and morning itchiness is the humble house dust mite. These microscopic arachnids thrive in warm, dark, slightly humid environments, making your child's mattress, duvet, and pillows their ideal habitat.
You can't see them, but millions of dust mites can populate a standard bed. It's not the mites themselves that cause the allergic reaction, but rather a specific protein found in their microscopic droppings. As your child tosses and turns during the night, these invisible particles launch into the air, settling directly onto the face, entering the nasal passages, and landing on the delicate conjunctiva. This continuous, night-long exposure is why many children with dust mite allergies wake up with severely swollen, red, and intensely itchy eyes every single morning. To understand the broader implications of this sensitivity, explore our comprehensive article on Dust mite allergy, which, despite the URL, delves deeply into the mechanics of the allergic response affecting so many households.
Prolonged exposure to dust mite allergens doesn't just cause immediate discomfort — it actively weakens the natural resilience of the mucous membranes. When the conjunctiva is constantly battling indoor allergens throughout winter, it's left exhausted and highly vulnerable when spring pollen season arrives. This cumulative effect can make a child's overall allergy profile much more severe. Many parents wonder about the origins of these sensitivities and ask, Is allergy hereditary? While genetics certainly play a substantial role in predisposing a child to atopy, controlling the immediate environment is the most effective way to manage symptoms.
The most robust method to protect your child's eyes during the night is to completely cut off the dust mites' food supply and prevent their allergens from reaching the bed surface. This is where advanced nanofabric technology makes a tangible difference. By encasing the mattress and bedding in tightly woven nanofabric, you create an impenetrable mechanical barrier. The pores in the nanofabric are so incredibly small that a dust mite — and crucially, its microscopic allergens — simply can't pass through. We highly recommend equipping your child's bed with a Kid's Fitted Sheet for Allergy Sufferers. This ensures your child sleeps on a pristine, allergen-free surface, allowing their immune system and sensitive eyes to rest and recover fully overnight. Because nanofabric is exceptionally breathable, it also wicks away moisture, preventing the damp conditions that allow mould and bacteria to flourish.
Protect your child's sleep with anti-allergy bedding
Effective Home Care, Treatments, and Soothing Remedies
When your child is suffering from an eye infection, providing immediate comfort is your top priority. The treatment strategy for conjunctivitis in children depends heavily on the root cause. For bacterial infections, a doctor will typically prescribe antibiotic eye drops or an antibiotic ointment. While drops are easier to administer during the day, ointments can be particularly useful at night because they stay on the eye longer and help prevent the eyelids from gluing shut by morning. With proper antibiotic treatment, a bacterial infection usually clears up within three to five days.
Viral conjunctivitis, much like a common cold, simply has to run its course. Antibiotics are completely ineffective against viruses. In these cases, the focus shifts entirely to symptom relief. You can apply cool, damp compresses over the child's closed eyes to reduce swelling and soothe the burning sensation. It's vital to use a fresh, clean cotton pad or cloth for every single application to avoid reintroducing the virus or spreading it to the other eye. Always wipe gently from the inner corner of the eye (near the nose) towards the outer corner.
For allergic conjunctivitis, the main goal is to remove the allergen from the child's environment and calm the overactive histamine response. Over-the-counter or prescription antihistamine eye drops can provide rapid relief from the intense itching. Additionally, keeping the eyes well-lubricated helps to flush out any microscopic allergens that have landed on the conjunctiva.
Regardless of the cause, maintaining a clean and lubricated eye is universally beneficial. Gentle, natural eye drops can work wonders in soothing irritation, washing away debris, and providing a protective layer of moisture over the inflamed tissue. We highly recommend keeping a bottle of Oculocin Propo Eye Drops, 10 ml in your family medicine cabinet. Formulated with natural ingredients like propolis, chamomile, and aloe vera, these drops are incredibly gentle on a child's sensitive eyes while offering powerful soothing properties. If you prefer a more sterile, single-use application to prevent cross-contamination between family members, the Oculocin Propo Eye Drops, 10 vials are an exceptionally convenient and hygienic alternative.
Soothing eye drops for irritated eyes
Essential Hygiene Practices to Prevent Spreading
If there's one thing every parent needs to know about infectious conjunctivitis in children, it's that it spreads with astonishing speed. A single infected child can easily pass the bacteria or virus to siblings, parents, and an entire classroom if strict hygiene protocols aren't immediately put in place. The main mode of transmission is direct contact — touching the infected eye discharge and then touching another person, or contaminating a shared surface.
To build a fortress against the spread of infection, rigorous handwashing is your most powerful weapon. Every household member must wash their hands thoroughly with soap and warm water frequently throughout the day, especially after applying eye drops or helping the child clean their face. It's absolutely crucial that the infected child has their own dedicated set of face flannels, bath towels, and hand towels. Don't allow anyone else in the family to use these items, and wash them on a hot cycle after every single use.

You should also change the child's pillowcase every single day until the infection has completely cleared. The pillowcase acts as a sponge for the infectious discharge during the night, and resting a healthy eye on a contaminated pillowcase is a guaranteed way to spread the infection from one eye to the other. In terms of school and nursery, most educational institutions have strict exclusion policies. Generally, a child with bacterial or viral conjunctivitis should be kept at home until they've been on antibiotic treatment for at least 24 hours, or until the heavy discharge has completely stopped, to protect the wider school community.
When Is It Absolutely Vital to Consult a GP?
While many cases of conjunctivitis in children can be managed safely at home with proper hygiene and over-the-counter soothing drops, it's not a condition to take lightly. The eyes are incredibly delicate organs, and a severe, untreated infection can lead to complications affecting the deeper structures of the eye, such as the cornea. Knowing when to bypass home remedies and seek immediate professional medical attention is a critical part of parenting.
You should schedule an urgent appointment with your GP or an eye specialist if you observe any serious red flags. If the child is complaining of severe, sharp pain in the eye — rather than just a mild scratchy or gritty feeling — this is a warning sign that the infection may have spread beyond the conjunctiva. Similarly, if the child reports that their vision has become blurry or cloudy, or if they're experiencing extreme sensitivity to light to the point where they can't open their eyes in a normally lit room, professional evaluation is mandatory.
If you've been administering prescribed antibiotic treatments for two to three days and there's absolutely no visible improvement in the redness or the volume of discharge, you must return to the doctor. This could indicate that the infection is viral rather than bacterial, or that the specific bacteria causing the issue are resistant to the prescribed antibiotic. Finally, if the swelling spreads beyond the eyelids and begins to puff up the surrounding facial tissue, or if the child develops a high fever, don't delay in seeking medical help.
Dealing with conjunctivitis in children is an inevitable rite of passage for almost every parent. While it can be messy, uncomfortable, and highly disruptive to your family's routine, it's usually a very manageable condition. By staying vigilant for the early symptoms, maintaining impeccable household hygiene, and using the right treatments and allergen-blocking bedding, you can help your child navigate the discomfort swiftly. Remember, a calm approach, a gentle touch, and the right medical guidance will soon have your little one looking at the world with clear, bright, and healthy eyes once again.
Frequently asked questions
Is conjunctivitis in children highly contagious?
Yes, both bacterial and viral forms are incredibly contagious. They spread very easily through direct physical contact with the infected eye discharge, or indirectly by touching contaminated items such as shared towels, unwashed pillowcases, or toys. Allergic conjunctivitis, however, is an immune response to environmental triggers and isn't contagious at all.
How long does a typical eye infection last in a young child?
The duration depends entirely on the cause. A bacterial infection typically lasts between seven to ten days if left untreated, but this timeframe is significantly reduced to about three to five days once proper antibiotic treatment begins. Viral infections can be more stubborn, often taking anywhere from one to three weeks to fully resolve. Allergic inflammation will persist for as long as the child remains exposed to the specific allergen.
Can my child safely attend school or nursery with an eye infection?
If the infection is bacterial or viral, your child should absolutely stay at home to prevent a wider outbreak. Most GPs recommend waiting until the child has been receiving antibiotic treatment for at least 24 hours, or until the thick, contagious discharge has completely ceased. If the redness is strictly due to an allergy, the child isn't contagious and can attend school normally.
What's the safest way to clean the crusty discharge from my child's eyes?
Always wash your hands thoroughly before and after cleaning. Use a clean cotton pad or a soft cloth dipped in cooled, boiled water. Gently wipe the closed eye starting from the inner corner (closest to the nose) and moving outward towards the ear. Never wipe back and forth, and always use a fresh cotton pad for each wipe to ensure you don't reintroduce bacteria into the eye.
Can household dust mites really cause my child's eyes to become inflamed?
Absolutely. Dust mites are one of the most common indoor triggers for allergic conjunctivitis in children. The microscopic proteins found in dust mite droppings become airborne and settle on the sensitive conjunctiva during sleep, leading to intense morning itchiness, redness, and swelling. Using specialist nanofabric bedding is a highly effective way to block these allergens and protect your child's eyes.