Imagine waking up in the early hours, tossing and turning because your entire body feels like it's on fire. You reach out to scratch, hoping for a fleeting moment of relief, but the sensation only intensifies. An itchy rash has taken over, and suddenly your skin feels like an enemy rather than a protective shield. Scratching provides no real comfort, your sleep is completely disrupted, and as the day progresses, the relentless urge to scratch drives you to the brink of despair. This isn't just a minor inconvenience — it's your body's way of sounding an alarm. Your skin, the largest organ in your body, is trying to tell you that something is fundamentally out of balance. What exactly triggers this frustrating condition, and more importantly, how can you soothe your irritated skin and reclaim your comfort? Let's explore the underlying causes and discover effective, long-lasting solutions.

Key takeaways if you're short on time
- Identify the root trigger, as an itchy rash can stem from hidden allergies, chronic skin conditions, or even psychological stress.
- Resist the overwhelming urge to scratch, because damaging the fragile skin barrier can easily lead to painful secondary bacterial infections.
- Adopt a gentle daily cleansing routine, using mild, natural products that clean without stripping away essential protective oils.
- Nurture your internal gut microbiome, since your digestive health directly influences the clarity, resilience, and calmness of your skin.
- Seek professional medical advice promptly, especially if the rash is accompanied by a fever, breathing difficulties, or is spreading rapidly.
Understanding the Symptoms: What Does an Itchy Rash Look Like?
An itchy rash that spans the entire body is a systemic, widespread reaction. Your skin responds to an internal or external stimulus by producing a massive eruption of red, inflamed patches, raised bumps, or textured irregularities that demand immediate attention. Unlike a localised irritation — perhaps a single insect bite on your ankle or a small patch of dryness on your cheek — this widespread affliction covers vast expanses of your body simultaneously, causing profound discomfort.
How does this phenomenon actually present itself? An itchy rash is a master of disguise and can take on numerous forms. In some instances, it manifests as a constellation of tiny, pinpoint red bumps that feel rough and sandpaper-like to the touch. In other cases, you might observe large, raised welts or irregular, fiery-red patches that seem to merge into one another across your torso and limbs. The surrounding skin typically becomes severely dehydrated, leading to flaking, peeling, or the formation of silvery scales. In the most severe scenarios, the intense inflammation can cause localised swelling and even the development of fluid-filled blisters that weep when accidentally ruptured.
However, the most distressing aspect is undoubtedly the relentless pruritus — the medical term for itching. The intensity of this sensation varies wildly from person to person and case to case. It might start as a mild, fleeting tickle that you can easily ignore, but it can rapidly escalate into an overwhelming, maddening compulsion to scratch that jolts you awake in the dead of night, leaving you exhausted and highly irritable the following day.
This is precisely where the vicious itch-scratch cycle begins. It's a biological trap. When you scratch an itchy rash, you temporarily overload the local nerve endings, providing a brief, deceptive illusion of relief. Yet simultaneously, your fingernails are creating microscopic tears in the fragile epidermis. This physical trauma prompts your immune system to release even more inflammatory chemicals, such as histamine, which makes the itch even more ferocious. These tiny abrasions also serve as open doors for opportunistic bacteria, potentially transforming a simple allergic reaction into a painful, weeping infection that could leave permanent scars.
The Most Common Causes of an Itchy Rash
To effectively combat this widespread discomfort, you need to play the role of a medical detective. Here is a detailed look at the most frequent culprits responsible for triggering an itchy rash across your entire body.
Allergic Reactions and Environmental Triggers
You probably know the scenario perfectly well: one day you feel absolutely fine, and the next morning you wake up covered in an intensely itchy rash. This is the classic hallmark of an allergic reaction, which remains one of the primary culprits when it comes to full-body skin eruptions. Sometimes, for reasons that aren't entirely understood, your immune system decides to mount a massive, disproportionate defence against substances you encounter every day and generally consider completely harmless.
Your daily diet is often the first suspect in this investigative process. It only takes a handful of peanuts, a slice of aged cheese, a single egg, or a seemingly innocent prawn to send a sensitive individual's immune system into absolute overdrive. Medications can be equally treacherous. Antibiotics prescribed to cure a lingering infection, non-steroidal anti-inflammatory drugs meant to soothe an aching joint, or even routine blood pressure medications can paradoxically trigger a severe, widespread itchy rash as an unintended and highly frustrating side effect.
Insect bites and stings can also have a profound impact. While most people recover from a wasp or bee sting with nothing more than a localised bump and a bit of swearing, individuals with heightened sensitivities can experience a severe systemic reaction, resulting in an itchy rash that spreads far beyond the initial site of the sting. The modern cosmetics industry is also a minefield of potential allergens. The artificial fragrances, harsh preservatives, and synthetic dyes lurking in your favourite commercial shampoos, body lotions, and antiperspirants possess the remarkable ability to transform a calm complexion into an inflamed, itching battlefield.
A quintessential manifestation of a severe allergic reaction is hives (medically known as urticaria). These present as raised, intensely itchy, inflamed welts that closely resemble the aftermath of falling into a patch of stinging nettles. They're notoriously unpredictable, capable of appearing anywhere on the body, changing shape, fading, and reappearing in entirely new locations within a matter of hours. If you want to understand more about maintaining optimal hydration during these difficult flare-ups, learning how to care for dry skin is an essential first step in your recovery journey.

It's absolutely crucial to remember that an allergic itchy rash can sometimes be the early precursor to anaphylaxis. This is a life-threatening medical emergency characterised by severe swelling of the airways, profound difficulty breathing, a sudden drop in blood pressure, and a rapid, weak pulse. If an itchy rash is accompanied by any of these alarming symptoms, you must contact emergency services immediately.
Chronic Skin Conditions and Autoimmune Disorders
An itchy rash isn't always a fleeting, one-off event triggered by a rogue prawn or a new laundry detergent. Frequently, it's the visible, daily manifestation of a chronic skin condition — a persistent companion that a patient must learn to manage over the long term.
Atopic dermatitis, commonly known as eczema, is like an uninvited guest who simply refuses to leave and constantly returns when you least expect it. This chronic inflammatory disease is characterised by severely dry, deeply itchy, and inflamed skin that can sometimes weep clear fluid when the barrier is significantly compromised. Whilst eczema typically favours the creases of the elbows, the backs of the knees, the neck, and the face, severe flare-ups can easily engulf the entire body in an unrelenting itchy rash. It's heavily linked to genetics and frequently appears in individuals who have a family history of asthma, hay fever, or environmental allergies. To help manage these symptoms naturally and restore the lipid barrier, many individuals turn to the Natural Nourishing Body Cream AtopCare 330 ml, which provides deep, soothing hydration without introducing harsh, synthetic irritants.
Another prevalent cause of a widespread itchy rash is psoriasis. This is a complex autoimmune disorder that essentially tricks the skin into accelerating its cell turnover rate. Instead of shedding normally over a month, skin cells multiply up to ten times faster than usual. The inevitable result is a build-up of thick, red, raised plaques covered with distinctive silvery-white scales. These plaques aren't only visually prominent but can also itch intensely, crack open, and bleed, causing significant physical discomfort. Whilst psoriasis typically targets the elbows, knees, and scalp, guttate psoriasis — a specific variant often triggered by a streptococcal throat infection — can cause a droplet-like itchy rash to erupt dramatically across the entire torso and limbs.
A somewhat less common, yet equally distressing condition is lichen planus. This inflammatory disorder presents as a cluster of intensely itchy, flat-topped, purplish bumps. Beyond the skin, lichen planus can also mount an attack on the scalp, nails, and even the mucous membranes inside the mouth, making it a particularly intrusive and difficult condition to manage daily.
Deep Hydration for Irritated Skin
Bothersome Infections: Viral, Bacterial, and Fungal
Occasionally, an itchy rash is the direct result of an invasion by microscopic intruders — organisms that see your skin as the perfect, nutrient-rich environment to set up camp and multiply rapidly.
Viral infections are classic culprits in this category. Diseases such as chickenpox, rubella, and measles are conditions typically associated with childhood, but they can and do strike adults, often with much greater severity and longer recovery times. These viral illnesses usually begin as a scattering of tiny red dots that rapidly evolve into intensely itchy, fluid-filled blisters. The urge to scratch a viral itchy rash can be so overpowering that it requires immense willpower to resist, yet scratching is strictly forbidden as it can lead to permanent pitting, scarring, and secondary infections.
Bacterial infections also play a highly significant role. Impetigo, for instance, frequently begins as small, red, irritated patches that quickly transform into delicate blisters. Once these blisters rupture, they leave behind characteristic honey-coloured crusts that are highly contagious. Another common bacterial issue is folliculitis, which is essentially an inflammation of the hair follicles. It presents as an itchy rash composed of small red bumps, often with tiny white pustules at the centre, clustering around areas where hair grows and experiences friction from tight clothing or shaving.
Fungi are another group of unwelcome visitors that can wreak absolute havoc on your skin. Tinea corporis, commonly referred to as ringworm (despite having absolutely nothing to do with actual worms), creates a highly distinctive itchy rash. It forms expanding red rings with a scaly, raised border and a relatively clear centre. Candidiasis, caused by an overgrowth of the Candida albicans yeast, thrives in warm, moist environments. It typically produces a fiery red, fiercely itchy rash in the folds of the skin, such as under the arms, beneath the breasts, or in the groin area.

Finally, there is scabies — a highly contagious parasitic infection caused by the microscopic mite Sarcoptes scabiei. These tiny arachnids physically burrow into the uppermost layer of the skin to live and lay their eggs. The resulting allergic reaction to the mites and their waste products causes an excruciatingly itchy rash that's notoriously worse at night, often destroying any chance of restful sleep. The pimple-like bumps and tiny burrow lines typically appear between the fingers, on the wrists, around the waistline, and in the armpits.
Changes in the Skin and Gut Microbiome
It might sound like something out of a science fiction novel, but your skin and digestive tract are home to trillions of microscopic organisms — bacteria, fungi, and viruses — that live with you in a complex, symbiotic relationship. Modern dermatological science is rapidly uncovering just how profoundly these tiny entities influence your overall health, particularly the condition and resilience of your skin.
When researchers examine individuals suffering from atopic dermatitis, they discover that their skin microbiome is vastly different from that of a person with healthy skin. Whilst a healthy complexion hosts a rich, diverse ecosystem of protective bacteria, patients with a chronic itchy rash exhibit a distinct lack of microbial diversity. Furthermore, their skin is frequently overrun by a specific pathogenic bacterium known as Staphylococcus aureus. This overpopulation actively drives inflammation, exacerbating the redness, swelling, and relentless itching that characterises the condition.
Even more fascinating is the revelation that the root of an itchy rash might actually lie deep within the digestive system. An imbalance in your intestinal flora — perhaps caused by a poor diet high in processed sugars, chronic stress, or a recent course of broad-spectrum antibiotics — can trigger a systemic inflammatory response that eventually manifests on the surface of the skin. This phenomenon is often visualised as a domino effect: the first domino falls in the gut, and the final domino crashes down on the skin. Consequently, medical professionals are increasingly focusing on the "gut-skin axis" as a vital component of dermatological health.
These recent discoveries are changing how medical professionals approach the treatment of an itchy rash. The use of probiotics — beneficial bacteria designed to restore harmony to your internal and external microbiomes — is becoming a mainstream recommendation. Some pioneering clinics are even exploring the possibility of topical microbiome transplants, transferring healthy bacteria directly onto the skin of patients suffering from severe eczema, mirroring the success seen with gut microbiome therapies.
Immune System Disorders and Imbalances
Your immune system is exquisitely designed to function as a highly trained, elite defence force, protecting you from illness and infection. However, sometimes this complex network makes a critical error in judgement. It may react with overwhelming force to a minor threat or, conversely, fail to mount an adequate defence. These subtle, internal miscalculations are frequently the hidden drivers behind an itchy rash that seemingly has no obvious external cause.
Recent scientific investigations have highlighted several intriguing correlations. In many individuals plagued by chronic, unexplained itching, blood tests reveal abnormally high levels of a protein known as Immunoglobulin E (IgE). IgE is a specific type of antibody that the immune system typically deploys to combat parasites and mediate severe allergic reactions. Intriguingly, these same patients often exhibit unusually low levels of another vital antibody, Immunoglobulin G (IgG), which is primarily responsible for neutralising common bacteria and viruses.

Researchers have also noted an abnormally low count of CD8 T-lymphocytes alongside an elevated presence of eosinophils — a type of white blood cell intrinsically linked to allergic responses and asthma. It's as if their immune system is locked in a permanent state of high alert, constantly scanning for non-existent threats and attacking the skin in the process.
These immunological anomalies can also be tied to broader autoimmune diseases, such as systemic lupus erythematosus. Whilst lupus is famous for producing a characteristic "butterfly" rash across the cheeks and bridge of the nose, it can also induce a widespread, highly photosensitive itchy rash across the entire body. In these autoimmune scenarios, the immune system fundamentally misidentifies the body's own healthy tissues as dangerous foreign invaders and launches a relentless, damaging assault against them.
Contact Dermatitis: The Perils of Everyday Products
Imagine deciding to switch to a new, heavily advertised brand of laundry detergent, only to wake up the following morning covered in an angry, red, itchy rash from head to toe. This is a textbook illustration of contact dermatitis — a localised or widespread inflammatory reaction triggered when the skin comes into direct physical contact with an irritating substance or an allergen.
Whilst irritant contact dermatitis is usually confined precisely to the area that touched the offending substance (such as your hands becoming red and cracked after using harsh household bleach without protective rubber gloves), allergic contact dermatitis can be far more unpredictable. In highly sensitive individuals, or when the allergen is dispersed over a wide area, the reaction can spread dramatically, resulting in a full-body itchy rash.
Common culprits include heavily fragranced laundry detergents and fabric softeners. These products are explicitly designed to leave chemical residues in the fibres of your clothing so they smell "fresh" for weeks. Unfortunately, for someone with sensitive skin, wearing these clothes means constant, all-day exposure to chemical irritants. Similarly, wearing tight, synthetic fabrics like polyester during hot, humid weather traps sweat and friction against the skin, creating the ideal environment for a widespread itchy rash.
Your daily shower routine could also be to blame. Luxurious bath foams, heavily scented body washes, and lotions packed with artificial dyes and harsh preservatives are frequent triggers. Even the jewellery you wear isn't entirely innocent; metals such as nickel, commonly found in belt buckles, watch straps, and inexpensive earrings, are notorious for causing severe allergic reactions.
What makes contact dermatitis particularly frustrating is the phenomenon of sensitisation. You can use the exact same brand of soap or wear the same necklace for years without any issues whatsoever. Then, suddenly and without warning, your immune system decides it's had enough, and you develop a severe itchy rash upon your very next exposure.

Other Essential Factors: Stress, Hormones, and Climate
An itchy rash can occasionally be attributed to less obvious, more insidious lifestyle and environmental factors. The climate, for instance, plays a massive role in skin health. During the harsh winter months, the combination of freezing outdoor temperatures and fiercely dry indoor central heating strips the skin of its natural moisture. This severely compromises the protective lipid barrier, leading to microscopic cracks, profound dehydration, and a highly reactive itchy rash. Conversely, the height of summer brings excessive sweating, which can block sweat ducts and cause prickly heat — a different but equally maddening type of rash.
Psychological stress is another significant factor. You've probably noticed that when you're under immense pressure at work or dealing with personal turmoil, your physical health takes a hit. Skin conditions are exceptionally sensitive to emotional distress. Stress triggers the adrenal glands to flood the body with cortisol and other hormones, which can induce a cascade of inflammatory responses. It's no coincidence that individuals suffering from eczema or psoriasis frequently experience their most severe flare-ups during periods of high anxiety.
Hormonal fluctuations also deserve a prominent mention. Significant life events such as pregnancy, the monthly menstrual cycle, or the onset of menopause involve drastic shifts in oestrogen and progesterone levels. These hormonal rollercoasters can alter the skin's oil production, immune response, and overall sensitivity, sometimes resulting in a persistent itchy rash. Many women report that their skin becomes noticeably more irritable and prone to rashes during specific phases of their cycle.
Lastly, consider the irony of modern medicine. The very pharmaceutical drugs you take to cure one ailment can sometimes induce another. Antibiotics, blood pressure medications, non-steroidal anti-inflammatory drugs, and synthetic hormones all list a widespread itchy rash as a potential — and relatively common — side effect.
How to Diagnose the Root Cause of an Itchy Rash
When you finally decide to take your itchy rash to a medical professional, prepare yourself for a process that closely resembles a complex detective investigation. An itchy rash is much like a fingerprint; each eruption has its own unique visual characteristics, distribution pattern, and underlying narrative.
The consultation will invariably begin with a meticulous visual examination. Your dermatologist or GP will scrutinise your skin under bright lighting, observing the exact hue, shape, texture, and borders of the lesions. They may employ a dermatoscope — a specialised, illuminated magnifying instrument that allows them to peer beneath the very top layer of the skin, revealing microscopic structures and vascular patterns that are entirely invisible to the naked eye.
Following the physical exam is a comprehensive medical interview. The doctor will ask you numerous questions: When exactly did the itchy rash first appear? Is the sensation purely an itch, or is there an element of burning or pain? Does the itching intensify at a specific time of day, perhaps at night? What medications, supplements, or herbal remedies are you currently taking? Have you recently introduced a new food, changed your brand of washing powder, or started using a different body lotion? Do you have a family history of asthma, hay fever, or autoimmune disorders? Have you travelled internationally in the past month?
If the physician suspects an allergic origin, they'll likely recommend specialised allergy testing. Patch testing involves applying small adhesive squares containing various common allergens to your back. These are left in place for 48 hours to see if a delayed allergic reaction occurs. Alternatively, skin prick testing involves placing tiny drops of potential allergens on your forearm and gently puncturing the skin's surface. If you're allergic, a raised, red, itchy bump will appear within 15 minutes.
Blood tests are another crucial diagnostic tool. A full blood count can reveal elevated levels of eosinophils or specific IgE antibodies, both of which strongly point towards an allergic or parasitic cause. Furthermore, blood tests can identify inflammatory markers or specific autoantibodies that suggest an underlying autoimmune condition like lupus.
Should the doctor suspect a bacterial or fungal infection, they'll perform a simple skin swab. This sample is sent to a microbiology laboratory, where scientists will culture the specimen to identify exactly which microorganisms are flourishing on your skin, allowing for highly targeted antibiotic or antifungal therapy.
In particularly stubborn or ambiguous cases, the dermatologist may resort to a skin biopsy. This is a minor surgical procedure where a tiny piece of the affected skin — usually no larger than an apple seed — is removed under local anaesthetic. This tissue is then sent to a dermatopathologist, who examines the cellular structure under a high-powered microscope. A biopsy can definitively differentiate between various types of dermatitis, identify rare autoimmune blistering diseases, and rule out more sinister causes.
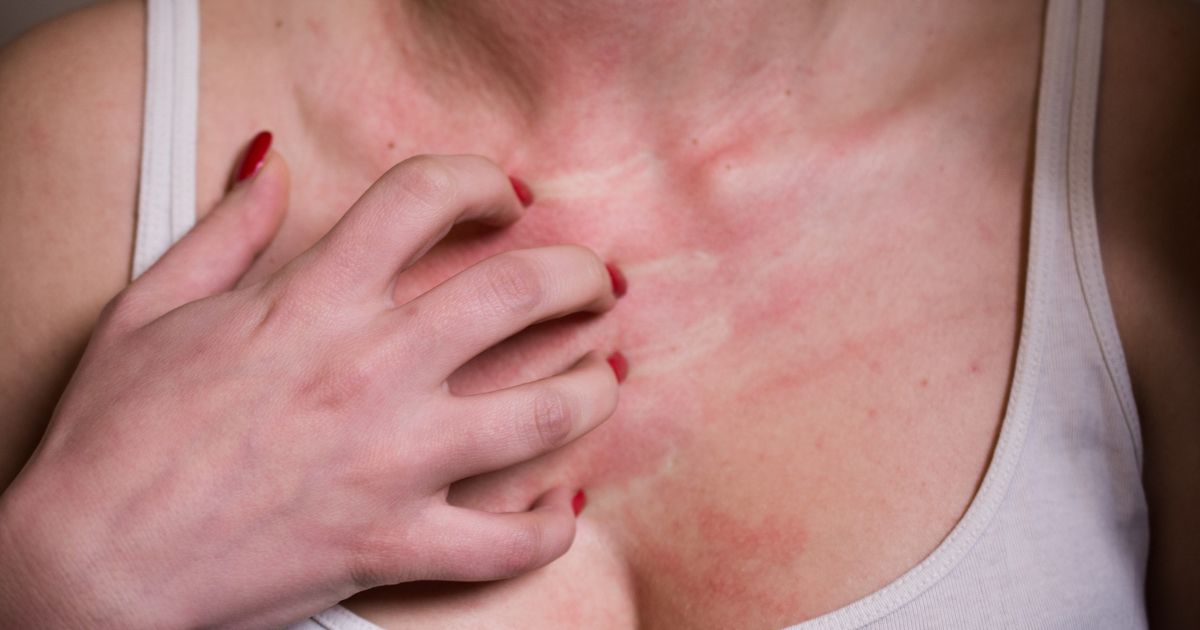
Effective Prevention Strategies for an Itchy Rash
Prevention is always better than a cure. This philosophy is especially pertinent when dealing with an itchy rash. Taking proactive steps to fortify your skin's natural defences is far easier and less painful than attempting to extinguish a massive inflammatory fire once it's already started. Let's explore the most effective preventative strategies.
Establishing a Gentle Skincare Routine
The absolute cornerstone of healthy, resilient skin is consistent, daily hydration. It may sound incredibly basic, but maintaining a regular moisturising regimen is one of the most powerful weapons in your arsenal against an itchy rash. The optimal time to apply a high-quality emollient is within three minutes of stepping out of the bath or shower, whilst your skin is still slightly damp. This technique locks in the ambient moisture, preventing it from evaporating into the dry air.
When it comes to cleansing, avoid harsh, brightly coloured, heavily perfumed soaps. These products strip the skin of its essential natural oils, leaving it vulnerable and prone to an itchy rash. Instead, opt for mild, soap-free cleansers that respect your skin's delicate acid mantle. For those with particularly reactive skin, incorporating the Natural Soap for Sensitive Skin AtopCare into your daily routine is an excellent choice. It cleanses effectively without causing dryness or irritation. Alternatively, for a lighter touch, the Moisturizing Cleansing Foam AtopCare 150 ml offers a soothing, airy lather that cleanses without disrupting your skin's delicate balance. To master the art of washing without causing damage, we highly recommend reading our detailed guide on proper skin cleansing techniques.
Your bathing habits also require careful consideration. Showers and baths should be kept brief — ideally under ten minutes — and the water temperature should be lukewarm, never scalding hot. Hot water is a notorious lipid-stripper; it literally melts away the protective fats that hold your skin cells together, paving the way for severe dehydration and an itchy rash. After bathing, gently pat your skin dry with a soft, clean towel. Never rub vigorously, as this friction alone is enough to trigger a histamine release and initiate a flare-up.
Finally, don't neglect sun protection. Ultraviolet radiation from the sun can severely exacerbate existing skin conditions, trigger photosensitive allergic reactions, and cause profound cellular damage. Applying a broad-spectrum sunscreen with a high SPF is non-negotiable, particularly if you're prone to an itchy rash.
Gentle Cleansing for Daily Care
Diet, Hydration, and Lifestyle Adjustments
Your skin is a direct reflection of your internal health, meaning that the food you consume has a profound impact on your complexion. A balanced, nutrient-dense diet is your first line of internal defence. Focus on incorporating foods rich in omega-3 fatty acids, such as wild-caught salmon, mackerel, chia seeds, and walnuts. Omega-3s possess potent anti-inflammatory properties that can help soothe an itchy rash from the inside out. Additionally, ensure you're consuming plenty of antioxidant-rich fruits and vegetables, which protect your skin cells from oxidative stress. If you're looking to support your skin's structural integrity further, exploring the best collagen for hair and skin can provide valuable insights into beneficial supplements.
Hydration is equally critical. Drinking adequate amounts of water ensures that your body can efficiently flush out toxins and maintain cellular plumpness. Aim for at least two to three litres of water daily, adjusting this amount based on your activity levels and the local climate.
Given the emerging science surrounding the gut-skin axis, nurturing your intestinal microbiome is a wise preventative strategy. Incorporating fermented foods like live-culture yoghurt, kefir, kimchi, and unpasteurised sauerkraut into your diet introduces beneficial probiotics into your digestive system. These "good" bacteria help regulate systemic inflammation, which can translate to a calmer, clearer complexion and a reduced risk of developing an itchy rash.

Lastly, managing psychological stress is paramount. Chronic stress elevates cortisol levels, which thins the skin, impairs barrier function, and triggers inflammation. Finding effective stress-reduction techniques — whether that involves daily mindfulness meditation, deep-breathing exercises, yoga, or simply taking regular walks in nature — is a critical component of preventing a stress-induced itchy rash.
Intelligent Clothing and Laundry Choices
The fabrics that sit directly against your skin for hours on end play a massive role in your dermatological health. If you're prone to an itchy rash, you must be highly selective about your wardrobe. Favour loose-fitting garments made from natural, highly breathable fibres such as organic cotton, bamboo, or high-quality silk. These materials allow air to circulate freely, preventing the accumulation of sweat and heat that can trigger irritation. Conversely, synthetic fabrics like polyester, nylon, and acrylic trap moisture and create a humid microclimate that fungi and bacteria absolutely love.
Your choice of laundry detergent is equally vital. Standard washing powders are often loaded with harsh surfactants, optical brighteners, and synthetic fragrances designed to mask odours. To a sensitive immune system, these chemicals are highly offensive. Switch to a hypoallergenic, fragrance-free liquid laundry detergent specifically formulated for sensitive skin. Furthermore, completely eliminate fabric softeners from your laundry routine. Whilst they make towels feel fluffy, they achieve this by coating the fibres in a thin layer of irritating chemicals — a guaranteed recipe for a widespread itchy rash. To be extra safe, always run your washing machine through an additional rinse cycle to ensure every last trace of detergent is washed away before you wear the clothes.
Optimising Your Indoor Environment
The environment inside your home can dramatically influence the likelihood of developing an itchy rash. During the colder months, central heating systems rapidly deplete the air of moisture, causing the relative humidity to plummet. This dry air acts like a sponge, pulling moisture directly out of your skin. To counteract this, invest in a high-quality humidifier for your bedroom and living areas, aiming to maintain an indoor humidity level between 45% and 55%.
You must also be vigilant about reducing indoor allergens. Dust mites, pet dander, and mould spores are microscopic triggers that can easily initiate an allergic itchy rash. Vacuum your home frequently using a machine equipped with a HEPA filter to trap fine particles. Encase your mattress and pillows in certified anti-dust mite covers, and wash your bedding weekly in hot water to eliminate any lingering allergens that could disturb your skin whilst you sleep.
When to See a Doctor About Your Itchy Rash
Whilst many instances of an itchy rash can be successfully managed at home with careful prevention and gentle skincare, there are specific scenarios where professional medical intervention is absolutely necessary. You should never ignore warning signs that suggest a more severe underlying condition.
You must seek immediate medical attention if your itchy rash is accompanied by systemic symptoms such as a high fever, severe joint pain, profound fatigue, or a general feeling of being unwell. These signs often point towards an active infection or a significant autoimmune flare-up that requires prescription medication.
Consult a doctor urgently if the rash spreads rapidly, begins to blister and peel over large areas of your body, or shows visible signs of bacterial infection, such as oozing yellow pus, radiating heat, or increasing tenderness. If an itchy rash appears shortly after you've started taking a new prescribed medication, contact your physician immediately, as this could be an adverse drug reaction.
Most importantly, if your itchy rash is accompanied by swelling of the face, lips, or tongue, a sensation of tightness in your throat, or any difficulty breathing, you must treat this as an absolute medical emergency. These are the classic symptoms of anaphylaxis, a severe and potentially fatal allergic reaction that requires immediate administration of adrenaline.
Dealing with an itchy rash that covers your entire body is undoubtedly a frustrating and physically demanding experience. It disrupts your sleep, shatters your concentration, and can severely impact your overall quality of life. However, by understanding the myriad of potential causes — from simple allergic reactions and contact dermatitis to complex autoimmune disorders and microbiome imbalances — you can begin to take control. Remember that patience is vital; identifying the exact trigger often requires a process of elimination and a bit of detective work. By adopting a meticulous, gentle skincare routine, making intelligent lifestyle and dietary choices, and knowing exactly when to seek professional medical advice, you can successfully soothe your irritated skin, banish the itch, and restore your body's natural harmony.
Sources
- GAWANDE, Atul. The itch. The New Yorker, 2008, 30: 58-65.
- KOBLENZER, Caroline S. Itching and the atopic skin. Journal of allergy and clinical immunology, 1999, 104.3: S109-S113.
- CHEE, Alvyn, et al. When life is an itch: What harms, helps, and heals from the patients' perspective? Differences and similarities among skin diseases. Dermatologic therapy, 2020, 33.4: e13606.
Frequently asked questions
Is a widespread itchy rash contagious?
It depends entirely on the underlying cause. Infections such as chickenpox or scabies are highly contagious and can be passed from person to person. However, if your itchy rash is caused by an allergic reaction, contact dermatitis, or a chronic condition like eczema, it's completely non-contagious.
Can psychological stress really cause an itchy rash?
Yes, absolutely. High levels of stress cause your body to release cortisol and other hormones that can trigger inflammation and weaken your skin's natural barrier. This can either worsen existing skin conditions or trigger a completely new stress-induced itchy rash.
How can I tell the difference between an allergic rash and an infection?
An allergic itchy rash typically appears very suddenly, often shortly after exposure to a trigger, and is intensely itchy. An infectious rash usually develops more gradually and is frequently accompanied by other systemic symptoms, such as a fever, fatigue, or general malaise. A doctor's diagnosis is required for certainty.
Can a food allergy cause an itchy rash all over my body?
Yes, food allergies can cause systemic reactions. Consuming an allergen like nuts, dairy, eggs, or seafood can trigger an immune response that results in a widespread itchy rash, often manifesting as hives, across your entire body.
How long does an itchy rash typically take to disappear?
The duration varies wildly depending on the cause. A mild allergic reaction may fade within a few hours or days once the allergen is removed. However, chronic conditions like psoriasis or severe eczema can persist for weeks, months, or even years, requiring ongoing management and care.





