You wake up in the middle of the night, and the first thing you do is scratch. Your arms, your back, your ankles — itchy skin refuses to let you sleep. In the morning, the mirror reveals reddened, irritated patches covered in scratch marks. Itchy skin is one of the most common dermatological complaints worldwide — according to the European Academy of Dermatology and Venereology, chronic pruritus affects up to 22% of the adult population. Yet most people only treat the symptom: they moisturise, scratch, or cool the area. They never look for the cause. Understanding why your skin itches is the first step towards genuine relief. In this article, we will walk through the 7 most common causes of itchy skin — from simple dryness through eczema to systemic diseases — and show you how to address each one effectively.

Key Takeaways if You're Short on Time
- Itchy skin affects up to 22% of the adult population, and its causes range from dry skin and allergic reactions to thyroid disorders and kidney disease.
- The most common culprit is a compromised skin barrier, which lets irritants in and moisture out — restoring the barrier is the foundation of every treatment.
- Vitamin E at a concentration of 5% demonstrably reduces itching by protecting skin lipids from oxidation and supporting the regeneration of the protective film.
- Oat oil contains avenanthramides, natural anti-inflammatory compounds that reduce itching and redness by up to 40% within two weeks of regular application.
- If itchy skin persists for more than six weeks without an obvious cause, see a dermatologist — it may be a sign of a systemic condition.
What Is Itchy Skin and Why You Cannot Afford to Ignore It
Itching — medically known as pruritus — is an unpleasant sensation that triggers the urge to scratch. At first glance, it seems trivial, but in reality it is a complex neurological process. The skin contains specialised nerve endings called pruriceptors that respond to histamine, proteases, cytokines, and other inflammatory mediators. When these receptors are activated, they send a signal to the brain, which interprets it as itching.
The real trouble starts when itchy skin becomes chronic. Scratching provides instant relief, but it simultaneously damages the skin — disrupting the skin barrier, creating micro-tears, and triggering an inflammatory cascade. This produces a vicious circle: itching leads to scratching, scratching leads to damage, damage leads to inflammation, and inflammation leads to even more intense itching. Dermatologists call this the "itch-scratch cycle," and breaking it is the cornerstone of successful treatment.
7 Causes of Itchy Skin and How to Address Them
1. Dry Skin (Xerosis) — the Most Common Culprit
Dry skin is responsible for itchy skin in more than 40% of patients who visit a dermatologist with this complaint. The mechanism is straightforward: when the skin loses moisture, it contracts, cracks, and exposes nerve endings. Those nerve endings then react to every stimulus — the friction of clothing, a change in temperature, even a draught of air.
Xerosis worsens in winter, when low outdoor humidity and overheated rooms drain the skin of its remaining moisture. But summer has its traps too — office air conditioning can dry the skin just as reliably as January frost. Long, hot showers and harsh cleansers that strip the natural skin film make things worse still.
How to treat it: The foundation is restoring and maintaining hydration. Shorten your showers to 5–10 minutes and lower the water temperature. Immediately after patting dry, apply an emollient — a cream or ointment that creates a protective film on the skin. Products containing vitamin E, which shields barrier lipids from oxidation, and oat oil, whose avenanthramides actively soothe itching, are exceptionally effective. We have covered what genuinely works for extremely dry skin in a separate article.
2. Atopic Eczema — When the Immune System Overreacts
Atopic eczema (atopic dermatitis) is a chronic inflammatory disease that affects 15–20% of children and 2–5% of adults in Europe. Itchy skin is its hallmark symptom — and it can be so intense that it disrupts sleep, concentration, and overall quality of life. The skin is dry, red, scaly, and may weep during acute flare-ups.
Behind eczema lies a combination of genetic predisposition (a mutation in the filaggrin gene — a protein essential for skin barrier function) and an exaggerated immune response. Atopic skin produces fewer ceramides and antimicrobial peptides, making it vulnerable to bacteria — particularly Staphylococcus aureus, which colonises up to 90% of eczematous skin and worsens both inflammation and itching.
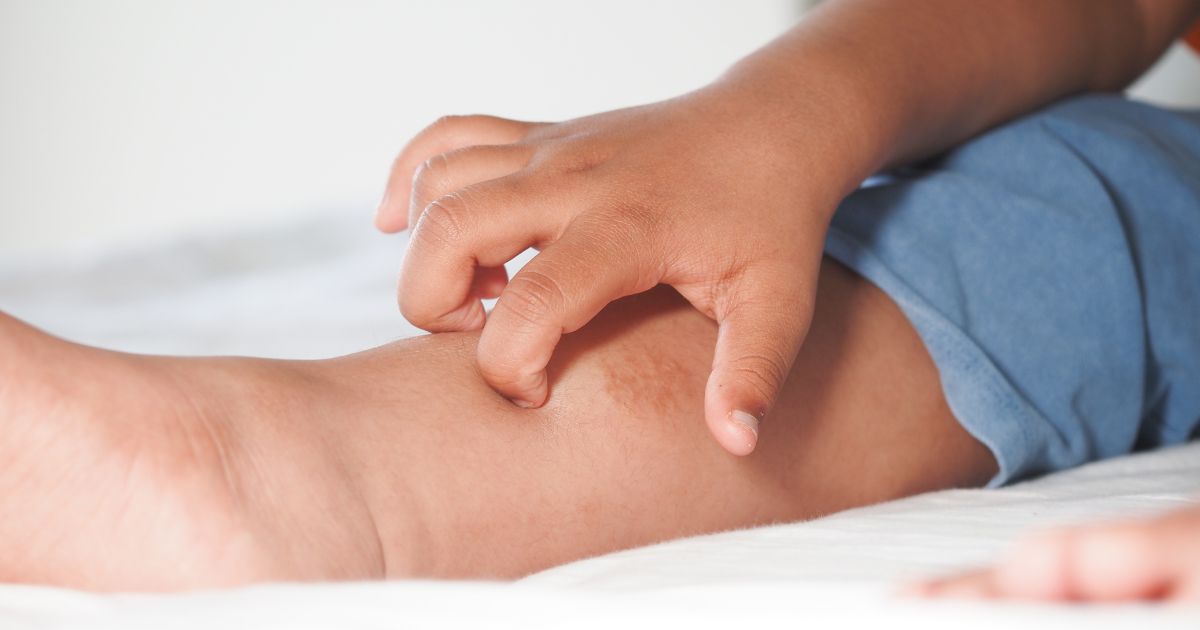
How to treat it: Regular emollients are the foundation — apply them at least twice a day, ideally right after bathing. Avoid known triggers (synthetic fabrics, fragrances, SLS). For a comprehensive overview of care strategies, take a look at our article on managing atopic eczema. Coconut oil has a special role in eczematous skin care — its component monolaurin demonstrates antimicrobial activity precisely against S. aureus, helping to break the cycle of infection and inflammation.
3. Contact Dermatitis — Your Skin Reacts to What It Touches
Contact dermatitis falls into two categories. Irritant contact dermatitis arises from direct chemical damage to the skin (cleaning products, solvents, disinfectants). Allergic contact dermatitis is mediated by the immune system and requires prior sensitisation. Both forms manifest as itching, redness, swelling, and blisters at the site of contact.
The most common contact allergens include nickel (jewellery, buckles, buttons), fragrances and preservatives in cosmetics, latex, cobalt, and formaldehyde. Irritant dermatitis is most frequently caused by detergents, wet gloves, repeated water exposure, and hand sanitiser gels. Occupational contact dermatitis affects up to 30% of healthcare workers and hairdressers.
How to treat it: Identify and eliminate the trigger — that is the single most important step. Then restore the damaged skin barrier with emollients rich in ceramides and vitamin E. Protect your hands by wearing cotton gloves under rubber gloves during wet work. Apply cooling compresses or an ointment with anti-inflammatory ingredients to intensely itchy areas.
4. Allergic Reactions — a Histamine Storm Beneath the Skin
When the body encounters an allergen — pollen, dust mite proteins, a food protein — mast cells in the skin release histamine. This causes vasodilation (widening of blood vessels), swelling, and activation of pruriceptors. The result is the classic triad: redness, swelling, and intense itchy skin. In urticaria (hives), raised, pale pink wheals also appear — they shift position and may merge together.
Allergic itching tends to be generalised — it affects the entire body, not just one spot. It often worsens at night, when cortisol levels (the body's natural anti-inflammatory hormone) drop and histamine levels rise. If itching is accompanied by breathlessness, tongue swelling, or dizziness, seek immediate medical help — it could be anaphylaxis. For distinguishing an allergic rash from other types, we recommend our article on itchy rashes and their causes.
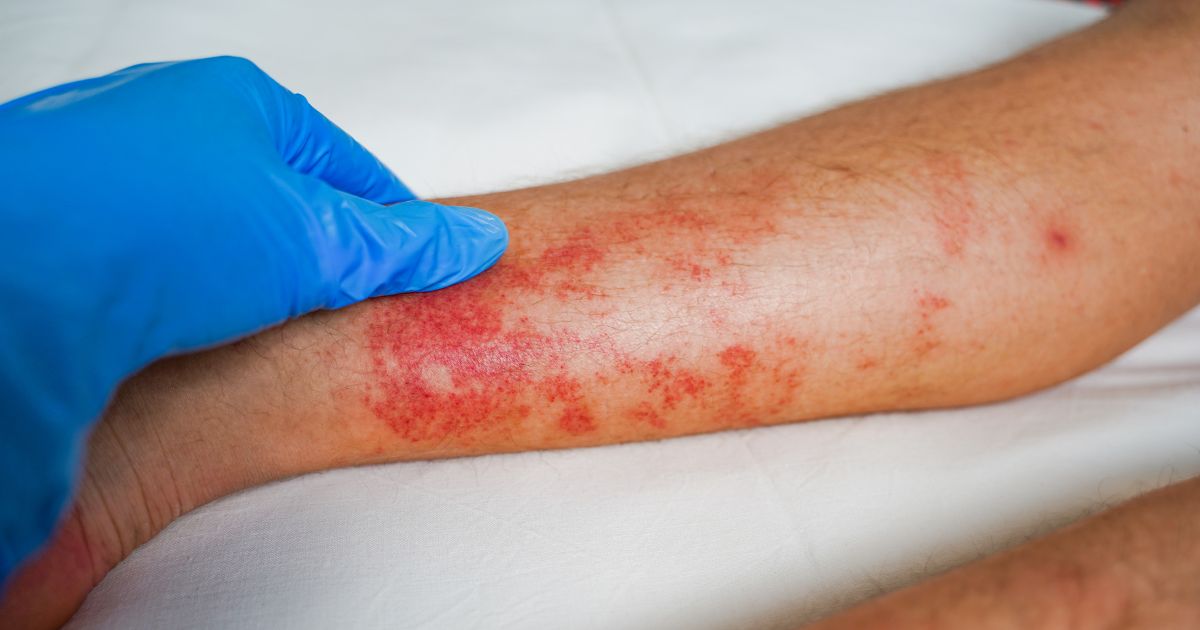
How to treat it: Antihistamines (cetirizine, loratadine) suppress acute itching. Cool compresses slow histamine release. Long-term, identifying the allergen (skin prick tests, specific IgE) and minimising contact is essential. After an allergic episode, regenerate the skin with emollients containing anti-inflammatory ingredients — oat oil and vitamin E help rebuild the barrier disrupted by inflammation.
5. Vitamin Deficiency — Itchy Skin as a Signal From Within
Itchy skin can be the first sign that your body is missing something essential. It is not merely about dryness from lack of water — specific deficiencies disrupt skin function at the cellular level.
Vitamin E is the primary fat-soluble antioxidant that protects the lipids of the skin barrier from oxidative damage. When levels are low, the lipid film on the skin surface degrades faster — the skin loses moisture and becomes prone to irritation and itching. Research has shown that topical application of vitamin E measurably reduces transepidermal water loss and alleviates pruritus.
Vitamin D regulates the proliferation and differentiation of keratinocytes — the cells that make up 90% of the skin. Its deficiency (common in 40–60% of the European population during winter months) is associated with worsening eczema, psoriasis, and non-specific itching. A study in the Journal of Allergy and Clinical Immunology showed that vitamin D supplementation reduced the severity of atopic dermatitis by 40% over three months.
B vitamins — particularly niacin (B3), pyridoxine (B6), and biotin (B7) — play a role in the metabolism of fatty acids that are essential for healthy skin. Niacin deficiency causes pellagra with its characteristic dermatitis, while biotin deficiency leads to seborrhoeic rash and itching around the mouth and nose.
How to treat it: If you suffer from long-term itchy skin without an obvious external cause, ask your doctor for blood tests checking vitamin D, E, and B group levels. Internally, enrich your diet with foods high in these vitamins (nuts, avocado, oily fish, eggs). Externally, choose products with a high concentration of vitamin E — studies indicate that a 5% concentration is optimal for protecting the skin barrier and relieving itching.

Editor's Pick
Regenerating Ointment with 5% Vitamin E AtopCare
An intensive ointment for itchy and irritated skin. The combination of 5% vitamin E, oat oil with avenanthramides, and coconut oil with monolaurin delivers a triple effect — it soothes itching, restores the skin barrier, and protects against bacterial infection. Free from parabens, silicones, and fragrance.
€10.00
View product6. Stress and Psychogenic Itchy Skin
Stress and the skin are more closely connected than most people realise. The skin and the nervous system both develop from the same embryonic germ layer (the ectoderm), which is why they communicate so intensely. During stress, the adrenal glands produce cortisol and adrenaline. In the short term, these hormones suppress inflammation, but under chronic stress the system becomes exhausted — cortisol levels drop and the immune system runs unchecked.
The result is increased production of pro-inflammatory cytokines in the skin, activation of mast cells, and release of histamine — even without any external allergen. Stress-related itching tends to be diffuse (all over the body), worsens in the evening and at night, and typically has no visible rash — the skin looks normal but itches unbearably.
How to treat it: Managing stress is just as important as skin care. Stress-reduction techniques (meditation, breathing exercises, regular physical activity) demonstrably lower the level of pro-inflammatory markers in the skin. Topically, cool compresses and emollients with soothing ingredients help. If itchy skin significantly impairs your quality of life, consider consulting a psychodermatologist — a specialist who understands the link between mind and skin.
7. Systemic Diseases — When Itchy Skin Signals a Bigger Problem
Chronic itchy skin without a visible rash may be a symptom of a more serious condition. Dermatologists call this "pruritus sine materia" — itching without skin findings. And that is precisely why it should never be taken lightly.
Thyroid disorders: Hypothyroidism (underactive thyroid) slows the skin's metabolism, reduces sebum production, and leads to dry, itchy skin. Hyperthyroidism, on the other hand, increases blood flow to the skin, causing sensations of warmth and itching. An estimated 10% of patients with chronic itching have an undiagnosed thyroid disorder.
Liver disease: Cholestatic itching — caused by the accumulation of bile acids in the blood — is one of the most intense types of itching. It typically affects the palms and soles of the feet, worsens at night, and does not respond to standard anti-itch medications. It occurs in hepatitis, cirrhosis, primary biliary cholangitis, and bile duct obstruction.
Kidney disease: Uraemic itching affects 40–70% of patients on dialysis. It is caused by the accumulation of uraemic toxins, calcium-phosphorus imbalance, and systemic inflammation. The itching tends to be generalised but most intense on the back.
How to treat it: If itchy skin lasts longer than six weeks, has no obvious skin-related cause, and does not respond to topical treatment, see your doctor. Routine blood tests (liver enzymes, creatinine, TSH, full blood count) can uncover hidden causes. Emollient care in the meantime helps ease symptoms and prevents further skin damage from scratching.
Why the Combination of Vitamin E, Oat Oil, and Coconut Oil Works on Itchy Skin
Each of these three ingredients tackles itching through a different mechanism — and it is precisely their combination that creates a synergistic effect more potent than any single ingredient alone.
Vitamin E (5% concentration) acts as a guardian of the skin barrier. It neutralises free radicals that damage ceramides and cholesterol in the skin's lipid film. When this film remains intact, moisture stays inside and irritants stay outside — and itchy skin subsides. A study published in the Journal of Investigative Dermatology demonstrated that vitamin E reduces transepidermal water loss by 19% within two weeks of regular application.
Oat oil is unique thanks to its avenanthramide content — polyphenols found exclusively in oats. These molecules inhibit the activation of NF-kappaB, one of the primary inflammatory triggers in the skin. In practical terms, this means less redness, less swelling, and less itching. Beyond that, oat oil stimulates ceramide production in the skin by up to 70%, actively rebuilding the damaged barrier.
Coconut oil adds an antimicrobial dimension. Its principal component — lauric acid — is converted in the skin into monolaurin, which disrupts bacterial cell membranes. This is particularly valuable for eczematous skin, where S. aureus colonises up to 90% of the surface and its toxins worsen itching. A study in the journal Dermatitis confirmed that coconut oil reduced S. aureus colonisation by 95% in patients with atopic eczema.
This triple combination in the nanoSPACE Cosmetics AtopCare range offers a comprehensive solution for itchy skin — it protects the barrier, suppresses inflammation, and fights bacteria simultaneously. This is an approach that does not merely treat the symptom but targets the root causes of itching.
Practical Tips for Immediate Relief From Itchy Skin
Before long-term care takes effect, you need to manage acute itching. Here are the methods dermatologists recommend for instant relief — ranked from most effective.
- Cool compresses — a cold, damp flannel placed on the itchy area for 10–15 minutes slows nerve signal conduction and reduces histamine release.
- Tapping instead of scratching — gently tapping the itchy spot with your fingertips activates touch receptors that "override" the itch signal without damaging the skin.
- Emollient from the fridge — store your ointment or cream in the refrigerator; the cooling effect on application doubles the soothing benefit.
- Cotton gloves at night — they protect the skin from unintentional scratching during sleep, when you have no control over the urge to scratch.
- Lukewarm (not hot) showers — hot water provides temporary relief but then paradoxically intensifies itching by dilating blood vessels and boosting histamine release.
For lasting relief, however, you need to address the cause. The Regenerating Ointment AtopCare with 5% vitamin E, oat oil, and coconut oil is formulated specifically for itchy skin — apply it to affected areas twice daily, ideally after showering onto slightly damp skin so the active ingredients are absorbed more effectively.
How to Care for Itch-Prone Skin — a Daily Routine
The right daily routine is the most powerful prevention tool you have. It is not complicated, but it requires consistency. Itchy skin is not a problem you solve once and forget — it is a condition you prevent every single day.
Shower in lukewarm water for no more than 5–10 minutes. Use gentle cleansers free from SLS, parabens, and synthetic fragrances. After showering, pat your skin dry with a towel — never rub. Within three minutes of drying, apply an emollient to your entire body. This short time window is critical — the skin is maximally hydrated after bathing and the emollient "locks" the moisture inside.
Apply AtopCare Hand Cream after every wash — hands are the most exposed part of the body and come into contact with the most irritating substances. For the rest of your body, use the AtopCare Body Cream, which, thanks to its lighter texture, covers larger areas and absorbs quickly without leaving a greasy film.
Choose clothing made from natural materials — cotton and silk are gentle on the skin, while wool and synthetics can worsen itching. Wash nightwear in fragrance-free detergents. And if you are curious about how itchy skin presents in stress-related rashes, take a look at our detailed article — stress is a common but under-discussed trigger.
Care for Itchy and Irritated Skin
Conclusion — Itchy Skin Is Not Just an Annoyance, It Is a Message
Itchy skin is telling you something. Sometimes the message is simple: "I am dry, I need hydration." Other times it is a warning: "Something inside your body is not working properly." And that is exactly why you cannot address it merely by scratching and hoping it will pass on its own.
Go through the seven causes we have described in this article and try to identify yours. Start with the basics — restore your skin barrier with a quality emollient containing vitamin E, oat oil, and coconut oil. Give your skin two to four weeks of consistent care. And if the itchy skin does not improve, or if it is accompanied by other symptoms, do not hesitate to visit a dermatologist. Your skin deserves it — and you deserve nights without waking and days without the constant urge to scratch.
Frequently Asked Questions
Why does my skin itch more at night than during the day?
At night, cortisol levels — the body's natural anti-inflammatory hormone — drop, while histamine levels rise. Transepidermal water loss also increases because body temperature rises slightly during the night. The combination of these factors makes itchy skin more intense in the evening and at night. Applying an emollient just before bed and keeping the bedroom temperature around 18–20 °C can help.
Can itchy skin be caused by a vitamin deficiency?
Yes, and significantly so. A vitamin E deficiency weakens the skin's lipid barrier, vitamin D deficiency worsens atopic dermatitis, and a lack of B vitamins (particularly niacin and biotin) manifests as dermatitis and itching. If you suffer from chronic itchy skin without an obvious skin-related cause, ask your doctor for blood tests checking these vitamins.
What is the best cream for itchy skin?
Look for products with anti-inflammatory and barrier-supporting ingredients — vitamin E (ideally at a 5% concentration), oat oil with avenanthramides, ceramides, and coconut oil. Avoid products containing fragrances, alcohol, and SLS, which worsen itching. An ointment is generally more effective than a cream, because it has higher occlusive capacity and retains moisture in the skin for longer.
When should I see a doctor about itchy skin?
See a dermatologist if the itching lasts longer than six weeks, does not respond to topical emollient treatment, is accompanied by unexplained weight loss, night sweats, or excessive fatigue, or if it appears without a visible rash. In such cases, it may be a symptom of a systemic condition — thyroid, liver, or kidney disorders.
How do I stop scratching when my skin itches?
The most effective technique is to replace scratching with a different sensation — tapping, pressing your palm against the area, or applying a cool compress. Keep your nails trimmed short. Wear cotton gloves at night. And above all, address the cause — regular application of an emollient with vitamin E and oat oil reduces itch intensity to the point where the urge to scratch gradually fades.

Sources
- Ständer, S. et al. (2007) 'Clinical classification of itch: a position paper of the International Forum for the Study of Itch', Acta Dermato-Venereologica, 87(4), pp. 291–294.
- Thiele, J. J. et al. (1998) 'Depletion of human stratum corneum vitamin E: an early and sensitive in vivo marker of UV induced photo-oxidation', Journal of Investigative Dermatology, 110(5), pp. 756–761.
- Reynertson, K. A. et al. (2015) 'Anti-inflammatory activities of colloidal oatmeal (Avena sativa) contribute to the effectiveness of oats in treatment of itch associated with dry, irritated skin', Journal of Drugs in Dermatology, 14(1), pp. 43–48.
- Verallo-Rowell, V. M. et al. (2008) 'Novel antibacterial and emollient effects of coconut and virgin olive oils in adult atopic dermatitis', Dermatitis, 19(6), pp. 308–315.
- Peroni, A. et al. (2012) 'Vitamin D and chronic urticaria/pruritus: a review', Indian Journal of Dermatology, 57(2), pp. 116–118.
- Matterne, U. et al. (2011) 'Prevalence, correlates and characteristics of chronic pruritus: a population-based cross-sectional study', Acta Dermato-Venereologica, 91(6), pp. 674–679.
- Nakatsuji, T. et al. (2009) 'Antimicrobial property of lauric acid against Propionibacterium acnes: its therapeutic potential for inflammatory acne vulgaris', Journal of Investigative Dermatology, 129(10), pp. 2480–2488.


