Your hands itch, crack, and sting every time you wash the dishes. The skin on your fingers is peeling, painful fissures form between the knuckles, and no chemist's cream lasts more than an hour. Hand eczema is one of the most common skin conditions in adulthood — roughly 10% of the population suffers from it, and in certain professions (hairdressers, healthcare workers, cleaners, chefs) the figure rises to one in three. And although it is not life-threatening, it can make life thoroughly miserable. Painful cracks make work difficult, shaking hands becomes an uncomfortable ordeal, and the constant itching disrupts both concentration and sleep. In this article, we will look at why hand eczema develops, what types exist, what makes it worse — and, most importantly, what actually works against it.
.jpg)
Key Takeaways if You're Short on Time
- Hand eczema affects approximately 10% of the adult population and comes in three main types — irritant contact, allergic contact, and dyshidrotic — with treatment depending on correct identification of the type.
- The most common triggers are frequent hand washing, chemicals, cold, and low humidity, which damage the skin barrier and set off a vicious circle of inflammation and itching.
- The cornerstone of treatment is restoring the skin barrier with emollients, which need to be applied at least 5–8 times a day — after every wash and before bed.
- Vitamin E at a concentration of 5% demonstrably supports regeneration of damaged skin, reduces inflammation, and protects ceramides in the skin barrier from oxidative damage.
- If hand eczema does not respond to care within 2–3 weeks, a dermatologist visit is necessary — short-term corticosteroid treatment or phototherapy may be required.
What Is Hand Eczema and Who Is Most at Risk
Hand eczema (hand dermatitis) is an inflammatory skin condition that manifests as redness, itching, scaling, blisters, or painful fissures on the palms, backs of the hands, and fingers. Unlike eczema on other parts of the body, hands are subjected to far greater stress — dozens of washes a day, contact with cleaning products, and constant mechanical strain. That is precisely why hand eczema is so common and so difficult to treat.
The statistics speak clearly. According to European dermatological studies, hand eczema occurs at some point in the lives of 15% of the population, and at any given time roughly 10% of adults are affected. In occupations involving frequent contact with water and chemicals — healthcare workers, hairdressers, chefs, cleaners, mechanics — prevalence reaches 30%. Women are affected approximately twice as often as men, primarily because of greater exposure to water and cleaning products both at home and at work.
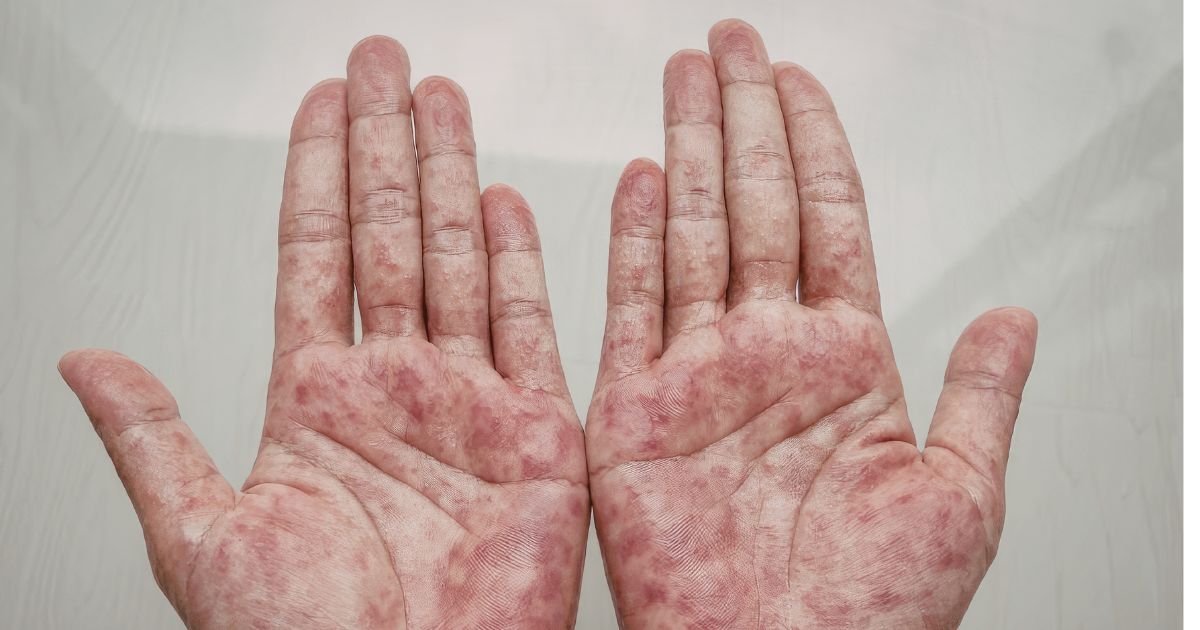
Three Main Types of Hand Eczema
The term "hand eczema" actually encompasses three distinct conditions that differ in cause, course, and treatment. Correct identification is critical — because what helps one type can make another worse.
Irritant Contact Hand Eczema
This accounts for up to 80% of all cases of hand eczema. It arises from direct damage to the skin barrier by irritating substances — water, soaps, disinfectants, cleaning products, food juices. It is not an allergic reaction but simply the consequence of repeated irritation. It presents as dry, red, cracked skin, most commonly on the backs of the hands and between the fingers. For healthcare workers who wash their hands 40–60 times per shift, it is practically an occupational disease.
Allergic Contact Hand Eczema
This results from an immune reaction to a specific allergen — nickel (jewellery, zips, coins), latex (gloves), preservatives in cosmetics (methylisothiazolinone), fragrances, or resins. Unlike irritant eczema, even minimal contact with the allergen is enough to trigger a reaction. It typically presents as itchy blisters, redness, and swelling at the contact site. Diagnosis requires patch testing by a dermatologist. If you suspect allergic eczema, our article on atopic eczema and how to manage it contains useful guidance on choosing the right care.
Dyshidrotic Hand Eczema
This manifests as tiny, intensely itchy blisters on the sides of the fingers, palms, and soles of the feet. The blisters are filled with clear fluid and, when they burst, leave painful, weeping patches. This type of hand eczema is often linked to stress, sweating, nickel contact, and seasonal fluctuations (worsening in spring and summer). You can read more in our detailed article on dyshidrotic eczema.
Why Hand Eczema Develops — the Barrier Damage Mechanism
Healthy hand skin is protected by the skin barrier, which consists of corneocytes (dead skin cells) held together by a lipid matrix — a mixture of ceramides, cholesterol, and free fatty acids. This barrier serves two purposes: it prevents water loss from the skin and keeps irritants, allergens, and microorganisms out.
When you wash your hands with soap, the surfactants dissolve not only dirt but also the barrier's protective lipids. A single wash will not destroy the skin — the barrier regenerates within 2–4 hours. The problem arises when washing is repeated before the barrier has time to recover. At 10–15 washes per day (a normal day in an office, nursery, or kitchen), the skin gradually loses its capacity for renewal. Water from deeper layers evaporates faster (transepidermal water loss rises), the skin dries out, cracks, and becomes permeable to irritants — which then trigger an inflammatory response.
This creates a vicious circle: compromised barrier, water loss, inflammation, itching, scratching, further barrier damage. The only way to break this circle is to actively rebuild the skin barrier from the outside — with emollients that replace missing lipids and lock moisture into the skin. We have written in detail about why barrier health is so fundamental in our article on extremely dry skin.
What Makes Hand Eczema Worse — Triggers You Can Avoid
Most people with hand eczema know they should avoid harsh cleaning products. But there are far more triggers — and some may surprise you.
Frequent contact with water is, paradoxically, one of the skin's greatest enemies. Even plain water without soap disrupts the lipid barrier. The rule is simple: the less water contact, the better. Always wear protective gloves during household chores — cotton gloves under rubber ones to prevent sweating.
Cold and low humidity dramatically worsen hand eczema. In winter, relative humidity in heated rooms drops below 25%, the skin loses moisture three times faster, and fissures deepen. Wearing gloves outdoors and using a humidifier indoors can make a visible difference.
Cleaning products and disinfectants contain surfactants and alcohol that aggressively dissolve skin lipids. Alcohol-based hand sanitiser gels dry the skin just as effectively as repeated soap washing.
Mechanical irritation — working with paper, cardboard, soil, concrete, or wood. Fine abrasive particles damage the skin surface and allow irritants to penetrate deeper layers.
Stress demonstrably worsens the course of eczema. Cortisol (the stress hormone) suppresses the immune response, slows healing, and disrupts ceramide synthesis in the skin barrier. For patients with stress-related eczema, dermatologists recommend relaxation techniques as part of the treatment. Cracked, irritated hand skin is often the result of a combination of stress and external irritating factors — you can read more in our article about dry hands and what helps.
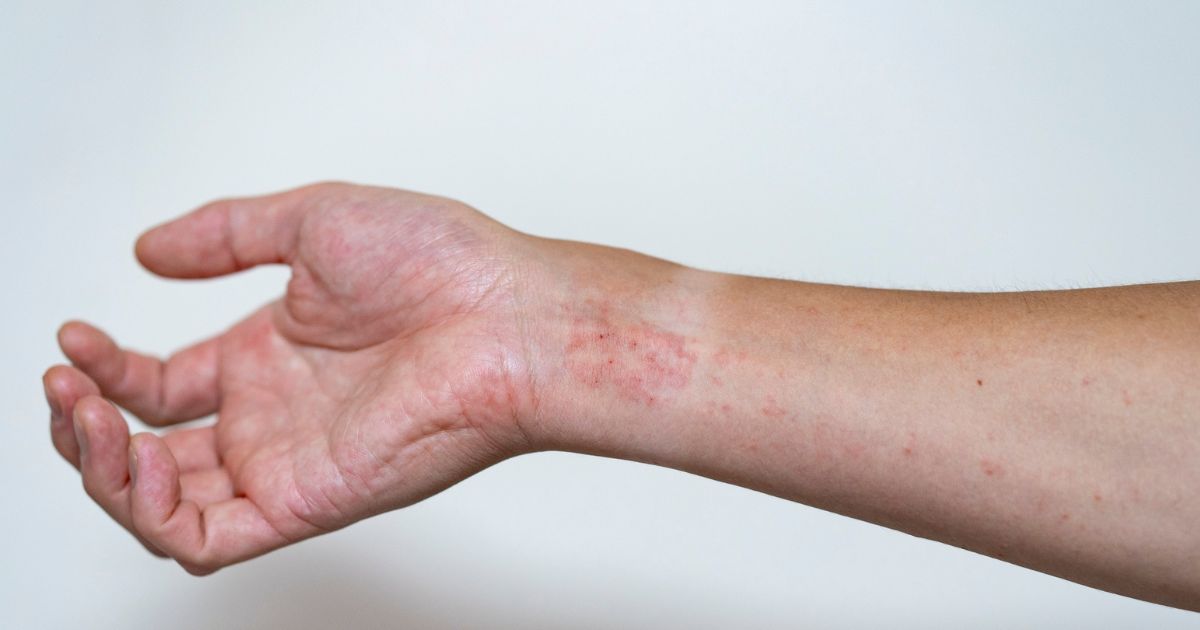
Hand Eczema in Specific Professions
Occupational hand eczema is one of the most common work-related skin conditions. In certain fields, the risk is so high that eczema becomes an almost inevitable career companion — unless preventive measures are adopted from the very start.
Healthcare workers wash and disinfect their hands 40–60 times per shift. A 2022 study published in Contact Dermatitis found that 30% of nurses suffer from hand eczema, rising to 45% among operating theatre staff. Alcohol-based sanitisers with added glycerine (gentler than soap washing) and consistent moisturising after every sanitisation are the solution.
Hairdressers combine three risk factors simultaneously — water, chemicals (dyes, bleaches, peroxides), and mechanical irritation. Hand eczema prevalence in this profession reaches 20–35%. Protective nitrile gloves during colouring and hair washing are an absolute baseline.
Food industry workers — chefs, bakers, butchers — face repeated contact with water, food juices (citrus acids, garlic, onion), spices, and cleaning products. Strict hygiene regulations demanding frequent hand washing further aggravate the skin.
How to Treat Hand Eczema — From Emollients to Dermatologist
Treatment of hand eczema rests on three tiers. Each has its place, and none can be skipped.
Tier One: Restoring the Skin Barrier
The foundation of all hand eczema treatment is regular, consistent moisturising. Emollients — softening products — replace missing lipids, soothe itching, heal fissures, and protect the skin from further irritation. Unlike the face or body, hands need moisturising far more frequently — at least after every wash and before bed, ideally 5–8 times a day.
When choosing an emollient for hand eczema, look for products containing ceramides, vitamin E, oat oil, or coconut oil. Avoid products with fragrance, parabens, silicones, and alcohol, which can further irritate already damaged skin. An ointment has an advantage over a cream for eczema — its higher fat content creates a more protective film and stays on the skin longer.
For overnight regeneration, the "wet wrap" technique is exceptionally effective: apply a thick layer of ointment to your hands, put on cotton gloves, and leave them on overnight. In the morning, you will be surprised at how markedly the skin has improved — fissures begin to close and itching subsides.
Tier Two: Anti-Inflammatory Treatment
If emollients alone are not enough and hand eczema persists beyond 2–3 weeks, it is time to see a dermatologist. The doctor may prescribe topical corticosteroids — modern preparations (mometasone, methylprednisolone) are safe even with longer-term use on the hands when applied correctly. The important thing is to follow instructions: apply only to affected areas, in a thin layer, for the recommended duration.
For patients who cannot or do not wish to use corticosteroids, alternatives exist — calcineurin inhibitors (tacrolimus, pimecrolimus), which suppress inflammation without the risks associated with corticosteroids. For severe hand eczema, a dermatologist may consider phototherapy (UVB light) or systemic treatment.
Tier Three: Identifying and Eliminating Triggers
No treatment will be effective long-term if you do not remove the cause. For allergic contact eczema, this is straightforward — patch tests reveal the allergen, and consistently avoiding it leads to symptom clearance. For irritant eczema, the situation is more complex, because the trigger is often the work itself. Protective gloves, switching to gentler cleaning products, and consistent skin protection throughout the day are measures that can bring hand eczema under control even without changing jobs.
Vitamin E and Hand Eczema — Why It Works
Vitamin E (tocopherol) is one of the most studied substances in dermatology, and its effects on damaged skin are supported by dozens of clinical studies. For hand eczema, it is particularly valuable because it acts on several levels simultaneously.
As an antioxidant, it protects ceramides and fatty acids in the skin barrier from oxidative damage. In eczematous skin, where the barrier is already compromised and exposed to free radicals from inflammation, this protection is especially precious. A study in the Indian Dermatology Online Journal confirmed that topical vitamin E at a 5% concentration significantly improves hydration of the stratum corneum and reduces transepidermal water loss.
As an anti-inflammatory agent, it suppresses the production of pro-inflammatory mediators — prostaglandin E2 and nitric oxide — that maintain the chronic inflammation of eczema. This means less redness, less itching, and faster healing of fissures.
As a healing accelerator, it speeds epithelialisation — the process in which new skin cells form and fissures close. A randomised study published in the Journal of Research in Medical Sciences demonstrated that vitamin E (400 IU daily orally) significantly improved eczema severity scores (SCORAD) compared to placebo.
In combination with oat oil, which stimulates ceramide production by 70%, and coconut oil with the antimicrobial effects of monolaurin, a synergistic effect emerges — the individual ingredients reinforce one another, and the outcome is better than the sum of their separate effects.

Editor's Pick
Regenerating Ointment with 5% Vitamin E AtopCare
An ointment developed specifically for dry, irritated, and eczematous skin. Just 9 ingredients — vitamin E, oat oil, coconut oil, ethyl ferulate, and hop extract. Free from parabens, silicones, fragrance, and alcohol. Ideal for overnight use under cotton gloves.
€10.00
View productCaring for Hands With Eczema — a Practical Guide
Theory matters, but you will beat hand eczema with daily habits. Here is what dermatologists recommend to their patients — and what genuinely works.
Washing your hands: Use lukewarm (not hot) water and gentle syndets without SLS instead of conventional soap. Dry your hands by gently patting with a towel — never rub. Within three minutes of washing, apply an emollient — during this window the skin is optimally prepared to absorb hydration.
Protection at work: When in contact with water and chemicals, wear two-layer gloves — cotton underneath (to absorb sweat) and nitrile or vinyl on top (to protect against chemicals). We do not recommend latex gloves — latex is a common allergen and can trigger or worsen hand eczema.
Overnight regeneration: Before bed, apply a thick layer of Regenerating Ointment AtopCare to your hands and put on cotton gloves. The skin regenerates intensively overnight, and the ointment under the gloves acts as an occlusive dressing — locking moisture and active ingredients into the skin.
During the day: Keep a hand cream within arm's reach at all times — in your pocket, your bag, on your desk, by the sink. The AtopCare Hand Cream is ideal for daytime use thanks to its lighter texture — it absorbs quickly and leaves no greasy film. At night, switch to the ointment for more intensive moisturising and protection.
Preventing flare-ups: Always wear gloves outdoors in winter, keep indoor humidity above 40%, and replace aggressive cleaning products with gentler alternatives. Every episode of hand eczema you prevent is better than one you have to treat.
Why Not All Creams Are Equal When It Comes to Hand Eczema
There are hundreds of products on the market that promise relief from eczema. But not all are created with equal care — and some may irritate the skin rather than soothe it. The more ingredients a product contains, the greater the risk that one of them will trigger a reaction on sensitive, eczematous skin.
The AtopCare range from nanoSPACE Cosmetics was built on the opposite philosophy: less is more. The Regenerating Ointment AtopCare contains just 9 ingredients — each with a clear purpose and none there unnecessarily. Vitamin E (5%) protects and regenerates, oat oil stimulates ceramide production, coconut oil provides antimicrobial action, ethyl ferulate amplifies the antioxidant effect of vitamin E, and hop extract calms inflammation. No parabens, silicones, fragrance, or alcohol.
For daily hand eczema care, the ideal combination is: AtopCare Hand Cream during the day (absorbs quickly, leaves no greasy film, so you can get straight back to work) and the ointment at night (higher fat content, more intensive protection, longer action). For whole-body care, the range also includes the AtopCare Body Cream, which is suitable for treating eczema that extends beyond the hands — onto wrists, forearms, or the crooks of the elbows.
Hand Eczema Care — Day and Night
When to See a Dermatologist
Mild hand eczema can be managed with emollients, hand protection, and lifestyle adjustments. But there are situations where a dermatologist visit is essential — and delaying it can make the condition significantly worse.
Hand eczema does not respond to care after 2–3 weeks of regular moisturising and protection. A topical corticosteroid may be needed to quickly suppress inflammation and allow the barrier to recover.
The skin is weeping, smells unpleasant, or has yellowish crusts. These are signs of bacterial superinfection, most commonly Staphylococcus aureus, which requires antibiotic treatment.
Blisters keep returning and worsen on contact with specific materials (jewellery, gloves, cosmetics). This points to a contact allergy, and patch testing is needed.
Eczema affects the nails — thickening, ridging, and colour changes of the nails can signal that hand eczema is transitioning into a chronic phase requiring more intensive treatment.
Eczema limits your work or daily activities. If fissures on your hands prevent you from working, typing, or managing your household, a dermatologist will help you put together a comprehensive treatment plan.
Conclusion — Hand Eczema Can Be Brought Under Control
Hand eczema is not a life sentence. It is a condition that demands understanding, patience, and the right habits — but it can be managed. The foundation is understanding what harms your skin and stopping it. Then consistently restoring the skin barrier with products that contain what the skin genuinely needs — vitamin E, ceramides, natural oils — and nothing that could irritate it. And if home care is not enough, do not hesitate to see a dermatologist. Modern treatment can bring even severe hand eczema under control. Your hands deserve it.
Frequently Asked Questions
How often should I moisturise hands with eczema?
At least after every hand wash and before bed — approximately 5–8 times a day. During the day, use a lighter cream that absorbs quickly and leaves no greasy film. At night, apply a thick layer of ointment and put on cotton gloves — the skin regenerates intensively overnight, and the occlusive dressing multiplies the product's efficacy.
Is hand eczema contagious?
No. Hand eczema is not an infectious condition and cannot be transmitted through contact, handshakes, or shared objects. It is an inflammatory reaction of the skin to irritants or allergens, or a manifestation of atopic predisposition. If anyone discourages contact because of your eczema, they are mistaken.
Can hand eczema clear up on its own?
It depends on the type. Acute irritant contact eczema can heal within 2–4 weeks if you stop irritating the skin and consistently moisturise. Chronic hand eczema requires long-term care — you cannot count on it disappearing by itself. Without treatment, it often worsens and progresses to lichenification (thickening of the skin), which is far harder to heal.
What is the difference between hand eczema and a fungal infection?
Eczema typically presents as symmetrical redness, itching, scaling, and blisters on both hands simultaneously. A fungal infection (tinea manuum) usually affects one hand, has a distinct raised border, and may spread to the nails. If you are unsure, visit a dermatologist — the distinction matters because the treatments are entirely different. Corticosteroid ointments that help eczema can actually worsen a fungal infection.
Can I use hand sanitiser if I have hand eczema?
Alcohol-based hand sanitisers dry the skin and can worsen eczema, especially if fissures are present (stinging, pain). If you need to sanitise, choose a product with added glycerine or an emollient component. Always apply an emollient immediately after sanitising. As a general rule, for hand eczema, alcohol-based sanitiser is actually gentler than soap washing — it paradoxically disrupts the lipid barrier less.

Sources
- Diepgen, T. L. et al. (2009) 'Management of chronic hand eczema', Contact Dermatitis, 60(Suppl 1), pp. 1–38.
- Agner, T. et al. (2020) 'Hand eczema: epidemiology, prognosis and prevention', Journal of the European Academy of Dermatology and Venereology, 34(Suppl 1), pp. 4–12.
- Keen, M. A., Hassan, I. (2016) 'Vitamin E in dermatology', Indian Dermatology Online Journal, 7(4), pp. 311–315.
- Javanbakht, M. H. et al. (2011) 'Randomized controlled trial using vitamins E and D supplementation in atopic dermatitis', Journal of Dermatological Treatment, 22(3), pp. 144–150.
- Thyssen, J. P. et al. (2022) 'Guidelines for diagnosis, prevention, and treatment of hand eczema', Contact Dermatitis, 86(5), pp. 357–378.
- Wollenberg, A. et al. (2022) 'European guideline (EuroGuiDerm) on atopic eczema', Journal of the European Academy of Dermatology and Venereology, 36(9), pp. 1409–1431.


