Have you ever looked in the mirror and noticed persistent, red, itchy patches covered in greasy, yellowish flakes? Perhaps they appear along your hairline, around the creases of your nose, or even on your chest. You wash your face and apply endless lotions, yet the frustrating cycle continues—often when you least expect it. If this scenario sounds all too familiar, you might be dealing with seborrhoeic dermatitis. This incredibly common yet frequently misunderstood chronic inflammatory skin condition affects millions of people worldwide, causing physical discomfort and significant emotional distress. While facing a chronic skin issue might sound daunting, there is no need to despair. Although it can't be entirely cured in the traditional sense, seborrhoeic dermatitis is highly manageable. With the right knowledge, a scientifically backed approach, and a tailored skincare routine, you can drastically reduce flare-ups and feel comfortable in your skin again. Let's explore what this condition actually is, how to identify it, the underlying factors that trigger it, and the most effective strategies to keep it under control.
Key takeaways if you're short on time
- Seborrhoeic dermatitis is a chronic inflammatory skin condition, affecting roughly 3–5% of the global adult population.
- The most common symptoms include red patches, greasy scales, and persistent itching, particularly in areas with a high concentration of sebaceous glands.
- It typically manifests on the scalp, face, chest, and within various skin folds, making targeted and gentle skincare absolutely vital.
- The central cause involves an overgrowth of Malassezia yeast, combined with a compromised skin barrier and an abnormal immune response.
- While it can't be permanently cured, it's highly manageable through the use of antifungal treatments, anti-inflammatory products, and a consistent skincare regimen.
What Is Seborrhoeic Dermatitis and Who Does It Affect?
Seborrhoeic dermatitis is a common, chronic inflammatory skin disorder that primarily targets areas of the body rich in sebaceous (oil-producing) glands. These glands produce sebum, the natural oil that keeps our skin lubricated and protected. However, when the delicate balance of the skin's ecosystem is disrupted, these sebum-rich zones become ground zero for inflammation. You'll most frequently find seborrhoeic dermatitis developing on the scalp, the face (particularly around the nose and eyebrows), behind the ears, on the upper chest, and occasionally in skin folds such as the armpits or groin. Statistically, this condition affects approximately 3–5% of the adult population, though dermatologists widely believe this is a significant underestimate. Many people simply assume they have standard dry skin or mild dandruff, and therefore never seek a medical diagnosis. In fact, the milder form of seborrhoeic dermatitis—what we commonly call everyday dandruff—is estimated to affect up to 50% of the global population at some point in their lives. Seborrhoeic dermatitis tends to peak during two distinct phases of life. The first occurs in infancy, typically within the first three months, when it is commonly known as "cradle cap". The second major peak occurs in adulthood, most commonly between the ages of 30 and 60. Interestingly, men are significantly more prone to developing the condition than women, which researchers believe is linked to the influence of male hormones (androgens) on sebum production. Certain underlying health conditions also dramatically increase the likelihood of developing severe seborrhoeic dermatitis. For instance, up to 85% of patients living with HIV/AIDS experience this skin issue. It's also notably more prevalent in people diagnosed with neurological conditions such as Parkinson's disease, and studies indicate it affects the Afro-Caribbean population at a slightly higher rate than the Caucasian population.

The Central Causes of Seborrhoeic Dermatitis
For decades, the exact mechanisms behind seborrhoeic dermatitis remained a puzzle for dermatologists. Today, while research continues to evolve, scientific consensus points to a complex interplay of several central factors rather than a single isolated cause. Understanding these factors is essential for effectively managing the condition. The most prominent culprit is a genus of naturally occurring yeast known as Malassezia. This yeast resides peacefully on virtually everyone's skin, forming a normal part of the microbiome. However, in people prone to seborrhoeic dermatitis, this yeast behaves opportunistically. Malassezia feeds directly on the lipids (fats) found in our sebum. As it digests these oils, it leaves behind by-products, primarily oleic acid. For many people, oleic acid is harmless. But for those with seborrhoeic dermatitis, this acid penetrates the top layer of the skin, triggering a strong inflammatory immune response. The body perceives the oleic acid as an invader, leading to the rapid shedding of skin cells, redness, and the formation of those characteristic greasy flakes. Beyond the yeast itself, a compromised epidermal barrier plays a crucial role. When skin cells don't form a tight, protective seal, moisture escapes easily, and external irritants—including the by-products of Malassezia—can penetrate deeply. This is why incorporating a high-quality, barrier-repairing product like the Natural Nourishing Body Cream AtopCare 330 ml into your daily routine is so important. By fortifying the skin's natural defences, you reduce the likelihood of irritants causing a severe flare-up. Genetics also play a significant role. Recent research has identified 11 specific genes associated with an increased risk of developing seborrhoeic dermatitis. These genes largely govern how the immune system functions and how the skin barrier is constructed. A 2024 study revealed that seborrhoeic dermatitis possesses its own unique genomic profile, officially classifying it as a distinct immune-mediated disease with mechanisms entirely separate from conditions like psoriasis or atopic eczema.
Essential Care for Sensitive Skin
Recognising the Symptoms: How to Tell If You Have Seborrhoeic Dermatitis
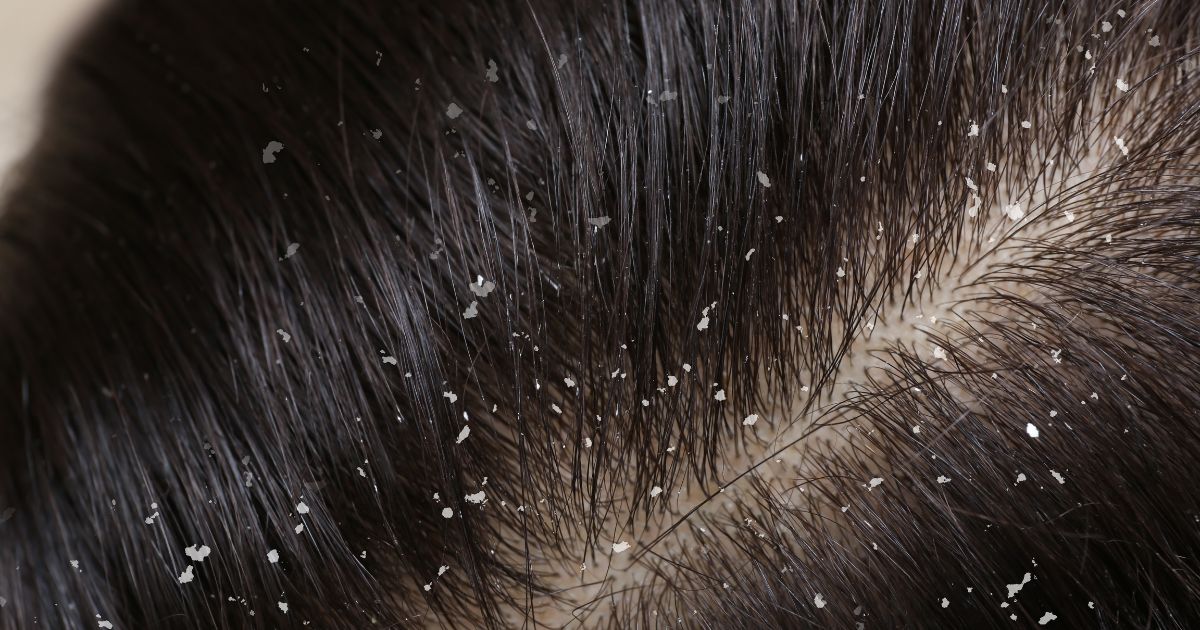
Because skin conditions often mimic one another, knowing the precise hallmarks of seborrhoeic dermatitis is vital for seeking the correct treatment. The symptoms typically present as a combination of distinct visual and physical cues. The most prominent sign is the appearance of red (erythematous) patches. In lighter skin tones, these patches often take on a salmon-pink or yellowish-red hue. These red areas are usually covered in scales or flakes. Unlike the dry, silvery scales of psoriasis, seborrhoeic dermatitis flakes are usually yellowish or white, and distinctly greasy to the touch. While not everyone experiences physical discomfort, itching and a mild burning sensation are very common, particularly when the scalp is heavily involved or when you're sweating. The condition is notoriously chronic and relapsing, meaning you'll likely experience periods of clear skin followed by sudden, frustrating flare-ups. The distribution of these patches on your body is a telling clue. On the scalp, it can range from mild, powdery dandruff to thick, adherent crusts that bind to the hair shafts. On the face, the redness and scaling tend to settle in the creases around the nostrils (the nasolabial folds), between and within the eyebrows, and along the hairline. It is also typical to find these greasy scales in and behind the ears. On the torso, lesions frequently form a petal-like or ring-like pattern over the breastbone, and occasionally between the shoulder blades. In people who are overweight or prone to heavy sweating, the condition often develops in the warm, moist environment of skin folds, such as the armpits, the groin, and beneath the breasts.

Seborrhoeic Dermatitis in Infants
When this condition strikes infants, usually between three weeks and three months of age, it's almost universally referred to as cradle cap. Parents will notice thick, greasy, yellowish-brown crusts forming on the baby's scalp. While it can look somewhat alarming to a new parent, the infant is rarely bothered by it. Unlike atopic eczema, which causes intense, sleep-disrupting itching for babies, cradle cap is generally asymptomatic and clears up on its own within a few months.
Seborrhoeic Dermatitis in Darker Skin Tones
It's crucial to note that seborrhoeic dermatitis presents differently depending on your skin's natural melanin levels. In people with darker skin tones, the classic "redness" is often absent. Instead, the affected patches may appear hypopigmented (lighter than the surrounding skin), hyperpigmented (darker), or take on a brownish, grey, or even purplish tint. These pigmentary changes can persist long after the active inflammation has been treated, which can be a significant cosmetic concern.
Differentiating Seborrhoeic Dermatitis from Other Skin Conditions
Self-diagnosis can be tricky, and many people spend years treating the wrong condition. Seborrhoeic dermatitis frequently masquerades as other dermatological issues. For instance, psoriasis also causes red, scaly patches, but the scales of psoriasis are typically thick, dry, and silvery-white, with very sharply defined red borders. Psoriasis also tends to favour the outer edges of the elbows and knees, whereas seborrhoeic dermatitis prefers the oily centre of the chest and face. Atopic dermatitis (eczema) is another common point of confusion. If you're reading about caring for dry skin, you'll note that eczema is characterised by extreme dryness, intense itching, and a strong association with allergies and asthma. Eczema scales are dry, never greasy. Rosacea, which also causes facial redness, usually presents with visible, broken blood vessels and acne-like bumps, but it completely lacks the flaky scaling seen in seborrhoeic dermatitis. Finally, fungal infections like ringworm (tinea) create circular, red patches that clear in the centre and spread outward at the edges, which is a different pattern entirely.
What Triggers or Worsens Seborrhoeic Dermatitis?
Even if you have your condition largely under control, certain triggers can cause an unexpected and aggressive flare-up. These triggers are generally divided into external environmental factors and internal physiological factors.
External Environmental Factors
The weather plays an enormous role in the severity of seborrhoeic dermatitis. Most sufferers notice a significant worsening of their symptoms during the cold, dry months of winter. The lack of ambient humidity, combined with the harsh transition between freezing outdoor air and dry, centrally heated indoor air, strips the skin of its protective moisture barrier. Conversely, sun exposure during the summer months often improves the condition, likely due to the mild anti-inflammatory and antifungal effects of ultraviolet light. The products you apply to your skin can also be major culprits. Harsh, alkaline soaps, heavily fragranced cosmetics, and alcohol-based toners can strip away natural lipids and irritate the epidermis. This is precisely why understanding how to cleanse skin properly is so critical. Using a gentle, microbiome-friendly cleanser like the Moisturizing Cleansing Foam AtopCare 150 ml ensures you remove excess oil and debris without provoking an inflammatory response. Additionally, living in highly polluted urban environments exposes the skin to microscopic particulate matter that generates oxidative stress, further worsening inflammation.
Internal and Lifestyle Factors
Your internal state is just as important as your external environment. Psychological stress and chronic fatigue are universally recognised as two of the most potent triggers for a flare-up. When you're stressed, your body produces high levels of cortisol, which can alter your immune response and increase sebum production. Hormonal fluctuations also play a part, which explains why the condition often worsens during puberty or periods of hormonal imbalance. If you're already researching how to care for oily skin, you'll know that managing androgen levels is vital for controlling sebum. Certain medications can inadvertently trigger seborrhoeic dermatitis. Drugs that influence dopamine levels, powerful immunosuppressants, and lithium have all been linked to increased flare-ups. A weakened immune system, whether due to a temporary illness, extreme sleep deprivation, or a chronic condition, allows the Malassezia yeast to multiply unchecked. Interestingly, diet also has a measurable impact. A typical Western diet, heavy in processed foods, refined sugars, and unhealthy fats, promotes systemic inflammation. Conversely, recent dermatological studies have shown that a diet rich in fresh fruits and vegetables is associated with a 25% lower risk of developing severe seborrhoeic dermatitis.
Deep Nourishment and Barrier Repair
Effective Treatments to Manage Seborrhoeic Dermatitis
Because seborrhoeic dermatitis is a chronic condition, the goal of treatment isn't a permanent cure, but rather long-term control. Your approach will depend heavily on the severity of your symptoms and the specific areas affected. Generally speaking, dermatologists prefer to prescribe lighter formulations like shampoos, liquid solutions, gentle foams, and lightweight gels rather than heavy, occlusive ointments that can trap heat and sebum.
Antifungal Preparations
Since the Malassezia yeast is a central driver of the inflammation, antifungal agents are the cornerstone of medical treatment. Ketoconazole is perhaps the most widely used option. Available in creams and shampoos, it's highly effective at reducing the yeast population. Typically, it's used twice a week during an active flare-up, followed by a maintenance routine. Clotrimazole is another excellent antifungal that halts the growth of yeast, often combined with moisturising elements to soothe the skin. Other effective options include ciclopirox and zinc pyrithione, the latter being a staple ingredient in many over-the-counter anti-dandruff shampoos due to its dual antibacterial and antifungal properties.

Anti-Inflammatory Treatments
When the skin is severely red, swollen, and intensely itchy, antifungal treatments alone might not work fast enough. This is where anti-inflammatory agents step in. Topical corticosteroids are frequently prescribed for short-term use to rapidly calm the inflammation. They range from mild options, like hydrocortisone, which are safe for the face and for use in children, to very potent steroids reserved strictly for severe, stubborn plaques on the scalp or body. However, steroids must be used cautiously and exactly as directed, as prolonged use can lead to skin thinning and other adverse effects. For patients who need long-term anti-inflammatory control without the risks associated with steroids, topical calcineurin inhibitors (such as pimecrolimus and tacrolimus) are excellent alternatives. They modulate the immune response locally in the skin and are particularly useful for delicate areas like the face and eyelids.
Scale-Removing Agents
Before antifungal or anti-inflammatory creams can penetrate the skin effectively, the thick barrier of greasy scales must be removed. Keratolytic agents are designed exactly for this purpose. Salicylic acid is an effective, gentle exfoliant that dissolves the bonds between dead skin cells, allowing the flakes to wash away easily. Sulphur is another traditional remedy that boasts both anti-seborrhoeic and anti-yeast properties. Azelaic acid is also gaining popularity, as it helps normalise the production of skin cells while offering mild anti-inflammatory benefits.
Innovative Treatment Approaches
The field of dermatology is constantly evolving, bringing new hope to chronic sufferers. Recent clinical trials have demonstrated that combining Intense Pulsed Light (IPL) therapy with a topical application of 30% salicylic acid yields remarkable results for facial seborrhoeic dermatitis. The IPL helps to destroy the Malassezia yeast, reduce vascular redness, and limit sebum production. Furthermore, new topical medications like roflumilast are showing immense promise in clinical trials, offering high clearance rates without the side effects of traditional steroids. For those with severe, widespread, or treatment-resistant cases, doctors may occasionally prescribe oral antifungal tablets or even low doses of oral isotretinoin to dramatically shrink the sebaceous glands.

Daily Skincare Routines and Home Remedies for Seborrhoeic Dermatitis
Medical treatments are essential during a flare-up, but your daily habits dictate how often those flare-ups occur. Establishing a gentle, supportive skincare routine is your first line of defence. Avoid harsh, heavily fragranced soaps that strip your skin. Instead, opt for products specifically formulated for compromised barriers. Cleansing with the Natural Soap for Sensitive Skin AtopCare ensures that your skin is clean but not irritated. After cleansing, moisturising is critical, even if your skin feels oily. Dehydrated skin often overcompensates by producing even more sebum, feeding the yeast further. Use a lightweight, non-comedogenic moisturiser. For the body, applying the Natural Nurturing Body Oil AtopCare 200 ml while the skin is still slightly damp locks in hydration and provides essential lipids that help repair the stratum corneum. Internal support is just as vital as topical care. If you want to fortify your skin's structural integrity from the inside out, researching the best collagen for hair and skin can provide valuable insights into dietary supplements that support skin elasticity and barrier function. Additionally, taking a daily zinc supplement (around 5–15 mg) has been shown to support immune function and reduce skin inflammation. Finally, don't underestimate the power of stress reduction. Incorporating daily mindfulness, deep breathing exercises, or regular physical activity can lower cortisol levels, thereby reducing the hormonal triggers that lead to excess sebum and inflammation.
Conclusion
Living with seborrhoeic dermatitis can certainly be a test of patience. It's a chronic, relapsing condition that requires ongoing attention and care. However, it's entirely possible to achieve long periods of remission and maintain healthy, comfortable skin. By understanding the central causes, identifying the symptoms, avoiding your personal triggers, and combining medical treatments with a gentle, barrier-repairing skincare routine, you can take back control. Remember that everyone's skin is unique; what works perfectly for one person might require adjustment for another. Do not hesitate to consult a dermatologist to tailor a treatment plan specifically for you, and approach your daily skincare with consistency and care.
Frequently asked questions
What exactly is seborrhoeic dermatitis?
It's a common, chronic inflammatory skin condition that primarily affects areas of the body rich in sebaceous (oil-producing) glands. It typically presents as red, itchy patches covered in greasy, yellowish scales, most often appearing on the scalp, face, chest, and within skin folds.
How many people suffer from this skin condition?
Clinical seborrhoeic dermatitis affects approximately 3–5% of the global adult population. However, its milder form, commonly known as dandruff, is estimated to affect up to 50% of people at some point in their lives.
Who is most frequently affected by seborrhoeic dermatitis?
The condition generally peaks in two specific age groups: infants during their first three months of life (where it's known as cradle cap), and adults between the ages of 30 and 60. It's also notably more common in men than in women.
What are the primary causes of this issue?
It's caused by a combination of factors, primarily an overgrowth of a naturally occurring yeast called Malassezia, which feeds on skin oils. This is coupled with a compromised skin barrier, an abnormal immune response to the yeast, and underlying genetic predispositions.
Is seborrhoeic dermatitis hereditary?
While it is not directly passed down in a simple hereditary pattern, there is a strong genetic predisposition. Researchers have identified 11 specific genes related to immune function and skin barrier integrity that increase a person's likelihood of developing the condition.
Sources
- Arcutis Biotherapeutics (2024) 'New Research Reveals Genomic Profile of Seborrheic Dermatitis and Answers Key Questions on Immune Response and Skin Barrier Dysfunction', press release, 9 March.
- Földesová, J. (2018) 'Current trends in the therapy of seborrheic dermatitis', Dermatologie pro praxi, 12(4), pp. 173-176.
- Gu, R.L. and Wang, S.Q. (2020) 'Clinical study on treatment of facial seborrheic dermatitis with intense pulsed light combined with 30% supramolecular salicylic acid', Clinics (Sao Paulo), 75, p. e1875.





