Itching, redness, and scaly skin or pink patches - these are all possible manifestations of an allergic rash. One very common type is called hives or urticaria. Allergic reactions can be caused by many factors. Let's take a detailed look at what causes allergic rashes in both children and adults, and how they are treated.

Types of Allergic Skin Rashes
Skin allergies are among the most common types of allergic reactions addressed by allergists and dermatologists. Hands are particularly susceptible to allergic reactions, but they can manifest all over the body, including the genitals.
Skin allergies come in many forms, such as hives, allergic or contact dermatitis, and eczema. Each mentioned type has its specific clinical symptoms and treatment, but common symptoms include itching and burning of the skin. In more severe cases, there can be swelling and unsightly rashes.
Causes of Allergic Rashes
Allergic rashes are caused by the hypersensitivity of the immune system to various substances called allergens. These allergens can include:
- Foods such as peanuts, eggs, and milk.
- Dust mites, animal allergens, and pollen.
- Cosmetics, such as perfumes, creams, and deodorants.
- Medications, including antibiotics and aspirin.
- Metals, such as nickel and chromium.
- Latex.
People with atopic eczema, asthma, and rhinitis are more likely to become sensitive to certain substances and more prone to allergic rashes. Read our article on how to recognize allergies to learn more.
Appearance and Symptoms of Allergic Rashes
Allergic rashes can manifest in various ways, depending on their severity and cause. The most common symptoms include:
- Red or pink patches on the skin.
- Itching.
- Dry and scaly skin.
- Blisters or sores.
- Swelling.
Treatment of Allergic Rashes
The treatment of allergic rashes involves identifying and eliminating the allergen that is causing the problem. If the rash appears after taking medication, it may be necessary to stop using that particular drug. In the case of a rash caused by a specific food, it is important to identify and avoid consuming the triggering food. However, allergic rashes can also be caused by allergies to dust mites, pollen allergies, cats, or dogs. In such cases, it is important to use dust mite-proof bedding and air purifiers for allergy sufferers.
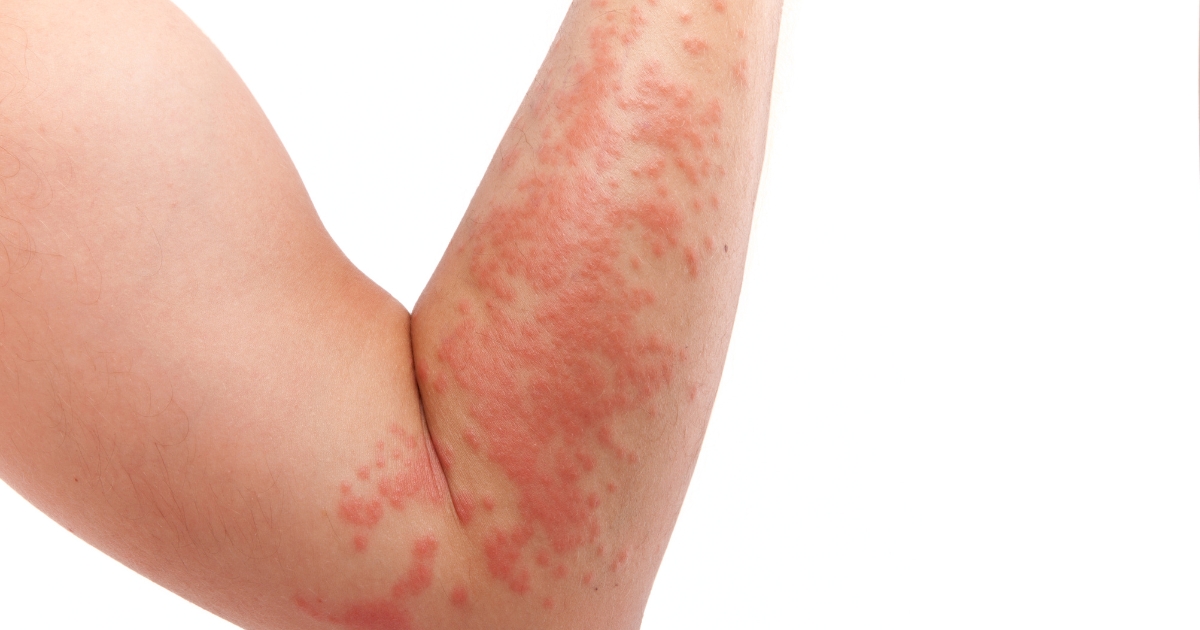
What is Hives?
Hives, also known as urticaria, is a type of skin condition characterized by itchy, red bumps. It is most commonly caused by an allergic reaction but can also occur due to other factors such as infections, stress, or certain medications. Hives typically appear suddenly and can last for a few hours to several days before resolving on their own.
The main symptom of hives is the development of raised, itchy welts on the skin. These welts can vary in size and shape and may merge together to form larger areas of swelling. They can appear anywhere on the body and may change in location and shape over time. In some cases, hives can be accompanied by other symptoms like swelling of the lips, face, or throat, difficulty breathing, or abdominal pain.
Treatment of Hives
The treatment of hives aims to relieve symptoms and identify and address the underlying cause. Here are some common approaches to managing hives:
-
Avoid triggers: If you can identify the trigger that is causing the hives, avoiding it is the first step. Common triggers include certain foods, medications, insect bites, pollen, and pet dander.
-
Antihistamines: Over-the-counter or prescription antihistamine medications can help reduce itching and inflammation associated with hives. Non-drowsy antihistamines like cetirizine, loratadine, or fexofenadine are often recommended.
-
Topical treatments: Applying cool compresses or taking cool showers can provide temporary relief from itching and soothe the skin. Calamine lotion or hydrocortisone cream may also help alleviate itching.
-
Avoid scratching: Scratching can worsen the symptoms and potentially lead to skin infections. It's important to resist the urge to scratch the affected areas.
-
Identify underlying conditions: If hives become chronic or recurrent, it's essential to work with a healthcare professional to identify any underlying medical conditions that may be contributing to the hives. This may involve further diagnostic tests or consultations with specialists.
-
Prescription medications: In severe cases or when hives do not respond to other treatments, a doctor may prescribe stronger medications such as corticosteroids or immune-suppressing drugs to control the symptoms.
-
Keep a symptom diary: If you're experiencing recurrent hives, keeping a record of your symptoms, potential triggers, and any other relevant information can be helpful. This can assist your healthcare provider in identifying patterns and potential triggers that may be causing your hives.
-
Allergy testing: If an allergic reaction is suspected as the cause of your hives, your healthcare provider may recommend allergy testing. This can help identify specific allergens that trigger your hives, allowing you to avoid them in the future.
-
Identify and manage stress: Stress can sometimes contribute to hives or exacerbate symptoms. Finding healthy ways to manage stress, such as practicing relaxation techniques, engaging in regular exercise, getting enough sleep, and seeking support from friends or professionals, may help reduce the frequency or severity of hives.
-
Avoid tight-fitting clothing: Wearing loose, breathable clothing can minimize friction and irritation to the skin, reducing the risk of hives. Avoiding tight-fitting clothes, particularly those made of materials that can cause sweating or irritation, can be beneficial.
-
Cold compresses: Applying cold compresses or ice packs to the affected areas can provide temporary relief from itching and reduce inflammation.
-
Consult an allergist or dermatologist: If your hives are persistent, recurrent, or significantly impacting your daily life, it may be helpful to consult with an allergist or dermatologist who specializes in skin conditions. They can provide further evaluation, recommend additional treatments or interventions, and offer expert guidance specific to your situation.
It's important to consult with a healthcare professional for an accurate diagnosis and appropriate treatment plan for hives. They can help identify the underlying cause and provide personalized recommendations based on your specific situation.
Remember, this information is not intended to replace professional medical advice. If you or someone you know is experiencing hives or any concerning symptoms, it's best to seek medical attention for proper evaluation and guidance.
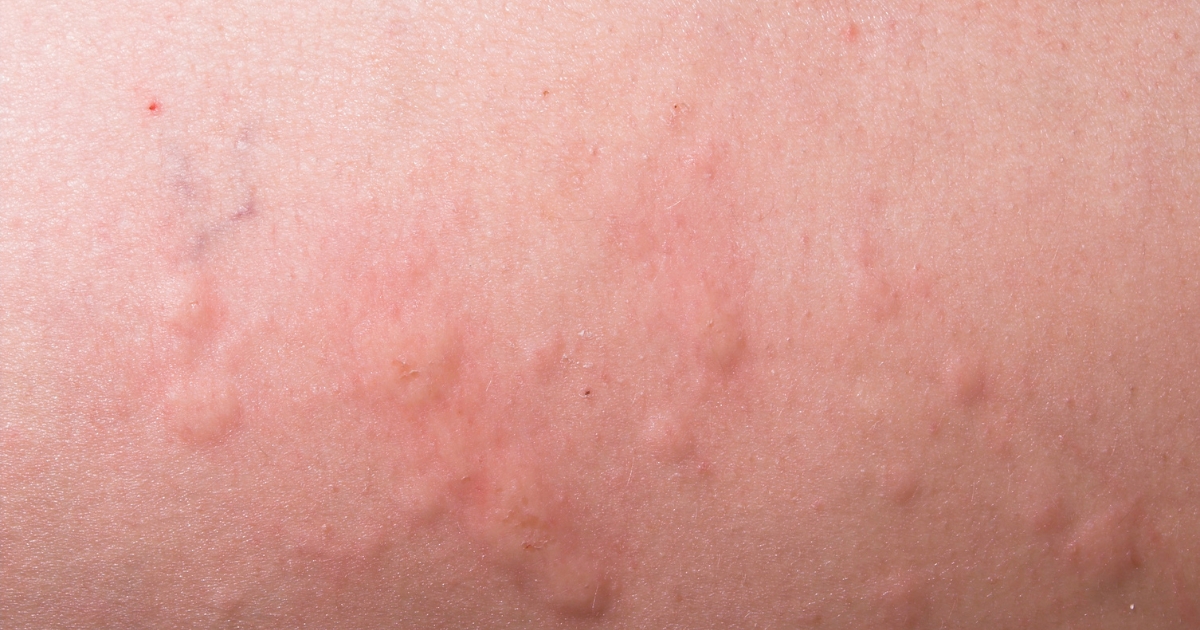
Rashes in Food Allergy
Food allergies can cause rashes and other symptoms such as swelling, itching, digestive issues, or breathing difficulties. Rashes caused by food allergies can take various forms, ranging from small bumps to extensive patches on the skin.
The most common food allergens are eggs, milk, peanuts, soy, fish, shellfish, and nuts.
If you suspect a food allergy, it is advisable to consult your doctor, who can refer you to an allergist for allergy testing. Once the allergy is confirmed, the doctor will determine appropriate treatment and dietary recommendations. In the case of a severe allergic reaction, such as anaphylactic shock, immediate medical attention is necessary.
Allergic Rashes in Children and Infants
Allergic rashes occur frequently in children and can be caused by an underdeveloped immune system or allergies. The most common cause is food allergies, pollen and dust mite allergies can also be factors. The rash appears similarly to that in adults, with red bumps that itch intensely. Read an article about allergies in children and infants.
FAQ
What causes hives?
Hives can be caused by various triggers, including food, pollen, dust mites, stress, temperature or pressure changes, infections, and certain medications.
How does hives appear?
Hives appear as red or white bumps surrounded by a reddened and intensely itchy area (wheals).
How is hives treated?
Treatment for hives includes the use of antihistamines, corticosteroids, and topical preparations to relieve itching. In some cases, immunosuppressants may be used. It is also important to avoid known triggers of hives.
How can I protect myself from hives?
You can protect yourself from hives by avoiding known allergens, using natural sun protection measures, dressing warmly in cold weather, and avoiding stressful situations.
What is the most common cause of hives in children?
The most common causes of hives in children are allergic reactions to food and insect bites. It can also occur as a secondary reaction to dust mites and pollen allergies. Less common causes include infections and autoimmune diseases.
Is hives hereditary?
There are genetic factors that can increase the risk of developing hives. If someone in the family has hives, their offspring may be more susceptible to this condition.
How long does hives last?
Hives can last from a few hours to several days. Depending on the cause and severity, the symptoms may be mild and transient or last for a longer duration.
Is hives contagious?
Hives are not contagious and cannot be transmitted to other individuals.
Is hives serious?
Most cases of hives are mild and do not require special treatment. However, in some cases, hives can be associated with serious symptoms such as facial and throat swelling, which can lead to breathing difficulties and anaphylactic shock. These cases require immediate medical attention.
What are the possible complications of hives during pregnancy?
Hives during pregnancy can be associated with complications such as breathing difficulties, impaired sleep quality, and breastfeeding difficulties after childbirth. It is important to consult with a doctor about appropriate treatment and monitor the development of hives during pregnancy.
Can citrus fruits cause allergic reactions?
Yes. Citrus fruits can be a strong allergen for some individuals, causing hives, swelling, itching, skin redness, swelling of the lips or eyes, digestive issues, and breathing difficulties.
How soon does an allergic rash appear?
An allergic rash can appear within minutes or hours after contact with the allergen.
Can I get a rash from a penicillin allergy?
Yes, a penicillin allergy can cause a skin rash. The rash can range from mild to severe, including small bumps, large flat patches, or generalized skin redness. In addition to the rash, other allergy symptoms may occur, such as itching, swelling, headaches, and even life-threatening allergic reactions like anaphylaxis. If you suspect an allergic reaction to penicillin, you should consult a doctor as soon as possible, who can provide appropriate treatment and recommend alternative medications if necessary.
How does an allergic rash appear in infants?
In infants, an allergic rash appears similarly to older children and adults, with itchy bumps that are white or red and surrounded by a red, itchy area. The skin may also be dry and scaly, and in some cases, swelling can occur. If you suspect your infant has an allergic rash, consult your pediatrician.
What can cause an allergic rash on the face?
An allergic rash on the face can be caused by various factors, such as food allergies, cosmetic allergies, or allergies to mites. It presents as red bumps, redness, itching, and sometimes dry skin. Headaches or nausea may also occur with a facial allergic rash. If you experience an allergic rash on your face, you can use various medications such as antihistamines or corticosteroids and avoid the allergens that trigger it.
Can hives be a symptom of COVID-19?
Studies have shown that hives can be one of the possible symptoms of COVID-19. According to one study, up to 20% of COVID-19 patients may experience skin symptoms, including hives. This manifestation often occurs in patients with mild symptoms or those who do not have other COVID-19 symptoms. Hives can also be the first or only symptom of COVID-19 in some patients. If a patient develops hives and there is suspicion of COVID-19, they should be tested for the coronavirus.
Can hives be a result of stress?
Yes, hives can be a result of stress. When a person experiences a stressful situation, histamine is released, which can cause skin rashes, including hives. Read about how to cope with stress.
Sources
- Greaves, M. W., & Kaplan, A. P. (Eds.). (2009). The urticarias: Advances in research and treatment. Springer Science & Business Media.
- Godfrey, S., & Rowe, B. (2015). Clinical paediatric respiratory medicine. CRC Press.
- Kettelhut, B. V. (2014). Urticaria: Clinical, diagnostic and therapeutic aspects. Springer.
- Zuberbier, T., & Grattan, C. (Eds.). (2010). Urticaria and angioedema. Springer Science & Business Media.
- Kanani, A., & Kastner, M. (2018). Food allergies: New research. Nova Science Publishers.
- Sharma, N., Singh, A., & Sharma, R. K. (2018). Urticaria: An updated overview. Indian journal of dermatology, 63(3), 168.
- Godse, K. V., Zawar, V., Krupashankar, D. S., & Girdhar, M. (2017). Urticaria: An Indian perspective. Indian Journal of Dermatology, 62(3), 237.
- Kaplan, A. P. (2008). Chronic urticaria: pathogenesis and treatment. Journal of Allergy and Clinical Immunology, 122(4), 644-650.
- Sánchez-Borges, M., Asero, R., Ansotegui, I. J., Baiardini, I., Bernstein, J. A., Canonica, G. W., ... & Greaves, M. W. (2015). Diagnosis and treatment of urticaria and angioedema: a worldwide perspective. World Allergy Organization Journal, 8(1), 1-18.
- O'Donnell, B. F., Lawlor, F., Simpson, J. G., & Greaves, M. W. (2002). The impact of chronic urticaria on the quality of life. British Journal of Dermatology, 146(6), 1074-1076.
- Jariwala, S., & Lakhani, S. (2018). Urticaria and angioedema. Allergy and Asthma Proceedings, 39(5), 343-345.
- Zuberbier, T., Asero, R., Bindslev-Jensen, C., Walter Canonica, G., Church, M. K., Giménez-Arnau, A. M., ... & Maurer, M. (2014). EAACI/GA2LEN/EDF/WAO guideline: definition, classification and diagnosis of urticaria. Allergy, 69(7), 868-887.
- Altrichter, S., Hawro, T., & Maurer, M. (2018). Urticaria and angioedema. The Lancet, 391(10119), 1096-1107.
- Kaplan, A. P. (2019). Urticaria and angioedema. In Allergy and Allergic Diseases (pp. 171-186). Springer, Cham.
- Sánchez-Borges, M., & Ansotegui, I. J. (2017). Diagnosis and treatment of urticaria and angioedema. World Allergy Organization Journal, 10(1), 1-10.

